The Link Between Gut Microbiome and Chronic Diseases
The gut microbiome is a complex community of microorganisms residing in the human intestinal tract. These microorganisms, including bacteria, viruses, fungi, and archaea, play a crucial role in maintaining overall health. Recent studies have highlighted the significant impact of the gut microbiome on chronic diseases such as obesity, diabetes, and cardiovascular issues. Alterations in the gut microbiota can lead to inflammation, metabolic disorders, and immune dysfunction. Therefore, understanding the dynamics of the gut microbiome is essential for preventing and managing chronic diseases. Factors such as diet, lifestyle, and medications can influence the composition of gut microbiota. Healthy eating habits rich in fiber, fruits, and vegetables can promote a balanced microbiome. Conversely, an unhealthy diet, high in sugar and processed foods, can disrupt this delicate balance. By fostering a diverse gut environment, we can enhance our immune function and prevent chronic conditions. Further research is needed to clarify the mechanisms that link gut microbiota to disease progression and to explore potential therapeutic interventions targeting the gut microbiome to combat chronic illnesses.
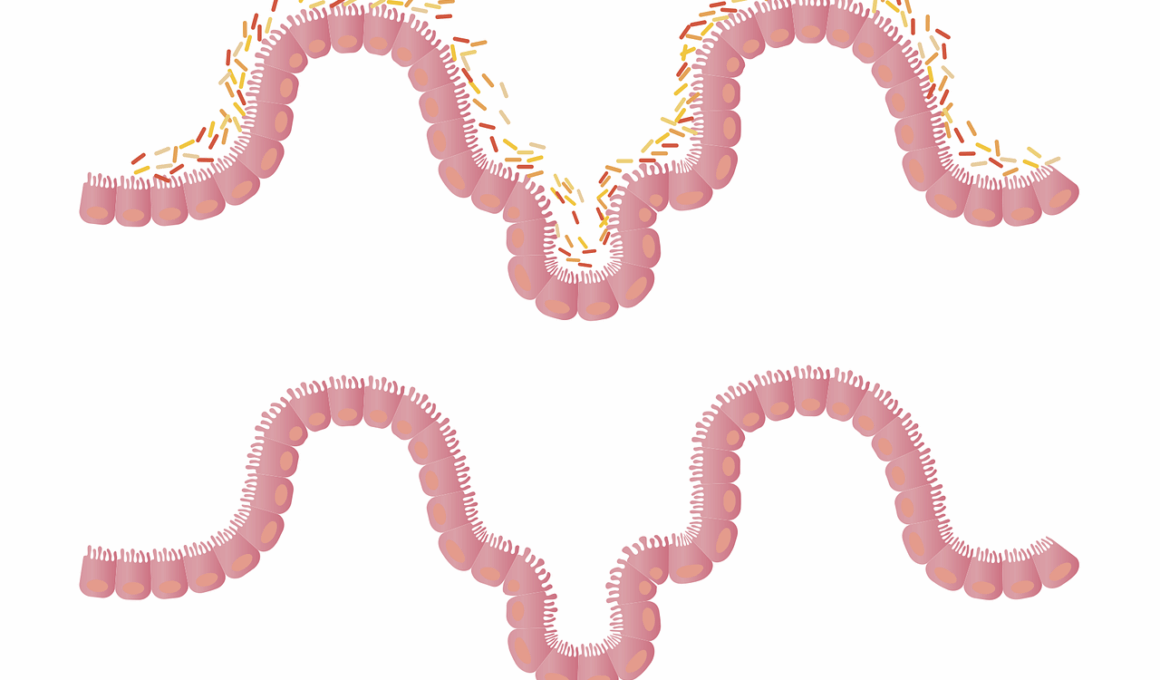
Chronic inflammation is a key player in the development of various diseases, and the gut microbiome is intricately linked to this process. When the gut microbiome is imbalanced, harmful bacteria can proliferate, leading to inflammation and disease. Dysbiosis, or microbial imbalance, can affect the gut barrier function, making it permeable and allowing toxins to enter the bloodstream. This can trigger systemic inflammation and exacerbate conditions like rheumatoid arthritis, inflammatory bowel disease, and even mental health disorders. Maintaining a healthy gut microbiome can help regulate inflammation and support digestive health. For instance, probiotics and prebiotics can help restore microbial balance, thus reducing inflammation. Probiotics introduce beneficial bacteria, while prebiotics serve as food for these good bacteria. Research continues to explore how specific strains of probiotics may hold promise in improving immune responses and decreasing inflammation. Additionally, dietary changes, such as increasing fiber intake and reducing processed foods, can significantly aid in restoring gut health. The intricate relationship between the gut microbiome and chronic inflammation indicates a promising avenue for therapeutic development that may improve patient outcomes and quality of life.
Gut Microbiome’s Role in Metabolic Health
The gut microbiome also plays a critical role in metabolic health. It is involved in various metabolic processes, including digestion, energy production, and storage of fat. Imbalances in gut bacteria can contribute to metabolic disorders, including obesity and insulin resistance. Some studies have indicated that individuals with obesity have a different gut microbiome composition than those with a healthy weight. For example, certain types of bacteria that encourage fat storage tend to be more prevalent in obese individuals. Moreover, these bacteria can also influence appetite regulation and energy expenditure. This relationship underscores the importance of gut health in managing weight and preventing metabolic syndrome. Understanding the gut-brain axis is also crucial, as gut bacteria can produce metabolites that affect our brain’s hunger signals. Therefore, specific dietary interventions, such as incorporating whole grains and fermented foods, can positively alter gut microbiota. This supports weight management and enhances metabolic health. Ongoing research aims to establish potential microbial biomarkers for obesity and diabetes, paving the way for personalized approaches in managing metabolic health through gut microbiome influences.
The gut microbiome’s relationship with the immune system highlights its importance in health and disease. The majority of the body’s immune cells are located in the gut, where they interact with various gut microbes. A balanced microbiome is essential for developing and maintaining an efficient immune response. Disruption of the gut microbiome can lead to immune dysregulation and increased susceptibility to infections and autoimmune diseases. For example, certain autoimmune conditions, like multiple sclerosis and systemic lupus erythematosus, have been linked to microbiome imbalances. Research has found that individuals with these conditions may have altered gut microbial profiles compared to healthy individuals. This connection suggests that microbiome-based therapies, such as fecal microbiota transplantation or targeted probiotics, may help modulate the immune response and potentially alleviate autoimmune symptoms. Furthermore, the gut microbiome can influence the effectiveness of vaccines, as a healthy gut flora can enhance vaccine efficacy by supporting immune activation. Thus, promoting gut health is not only crucial for preventing chronic diseases but also vital for optimizing immune function and response to infections and vaccinations.
Psychological Impacts of Gut Microbiome
Recent studies have established a fascinating link between gut microbiome health and mental well-being. This connection, often referred to as the gut-brain axis, shows how gut bacteria can influence brain function and moods. Imbalances in gut microbiota may play a role in conditions like anxiety, depression, and stress-related disorders. Gut bacteria produce neurotransmitters and metabolites, such as serotonin and gamma-aminobutyric acid (GABA), which affect mood and anxiety levels. Increased gut permeability can lead to neuroinflammation, further contributing to mental health issues. Thus, maintaining a healthy gut is essential for both physical and psychological wellness. Interventions such as dietary changes, prebiotics, and probiotics show promise in improving gut health and, in turn, mental health. Foods rich in omega-3 fatty acids, fermented products, and fibers can foster a diverse microbiome. To leverage this connection, future health strategies may involve targeted dietary recommendations and microbiome analysis in treating mental health disorders. As research continues to evolve, the pursuit of an optimal gut microbiome for better mental health will be an exciting frontier in healthcare.
Understanding the critical link between gut microbiome health and chronic diseases emphasizes the need for personalized nutrition and health strategies. Individual variations in microbiome composition can affect how different people respond to dietary changes or interventions. This highlights the importance of microbiome testing in developing tailored health plans. Personalized nutrition considers unique microbiome profiles and aims to optimize health outcomes through diet modulation. Incorporating a variety of foods can promote microbial diversity, thereby supporting overall health. Furthermore, establishing a healthy lifestyle, including regular exercise and stress management, can positively impact gut microbiota. As the research progresses, healthcare professionals increasingly recognize the gut microbiome’s central role in overall wellness. New technologies, such as microbiome analysis tools, can help individuals assess their gut health effectively. By understanding their unique gut profiles, people can adjust their diets to foster a healthier microbiome. This insight will help reduce the risks of chronic diseases, offering a pathway to better health. The intersection of microbiome research and personalized medicine then serves as a gateway to innovative solutions for managing and preventing chronic diseases in the future.
Future Directions in Gut Microbiome Research
Future research into the gut microbiome will likely focus on uncovering detailed mechanisms linking gut health to chronic diseases. Advancements in sequencing technology are improving our understanding of the microbial communities within the gut. This allows researchers to identify specific bacteria associated with health conditions and determine how they influence disease pathways. The application of artificial intelligence and machine learning may also revolutionize how we analyze microbiome data, revealing intricate patterns that connect gut health to various diseases. It may become possible to develop microbiome-based therapies tailored to individual gut profiles, optimizing treatment effectiveness. Other exciting areas of research will include exploring the potential of microbial metabolites and their effects on health. For instance, short-chain fatty acids produced by gut bacteria can influence inflammation and metabolic processes. Understanding these interactions may pave the way for novel therapeutic strategies. Additionally, by exploring dietary patterns and their influence on the microbiome, we can identify optimal nutrition strategies for chronic disease prevention. As the field evolves, a holistic approach that considers genetics, environment, and microbiome interactions will be crucial in shaping future healthcare paradigms.
In conclusion, the gut microbiome significantly influences chronic diseases, highlighting its role in health and disease management. Understanding this complex relationship is essential for developing effective strategies for prevention and treatment. Promoting gut health through diet and lifestyle changes can help restore microbial balance, potentially reducing the risk of chronic diseases. Utilizing probiotics, prebiotics, and personalized nutrition can further support gut well-being. As more research emerges, we’ll gain insights into the gut microbiome’s mechanisms, paving the way for innovative therapies tailored to individual needs. The gut microbiome also holds immense potential for improving mental health, alongside its physiological impacts. As we continue to uncover the complexities of the gut microbiome, we move toward an era of personalized medicine, focusing on holistic health approaches. By fostering healthy gut microbiota, we can enhance our overall well-being. Public health initiatives will play a pivotal role in educating individuals about the importance of gut health and its implications for chronic disease prevention. Engaging the community in discussions regarding gut health can lead to a proactive stance on wellness and motivate positive lifestyle changes that benefit future generations.