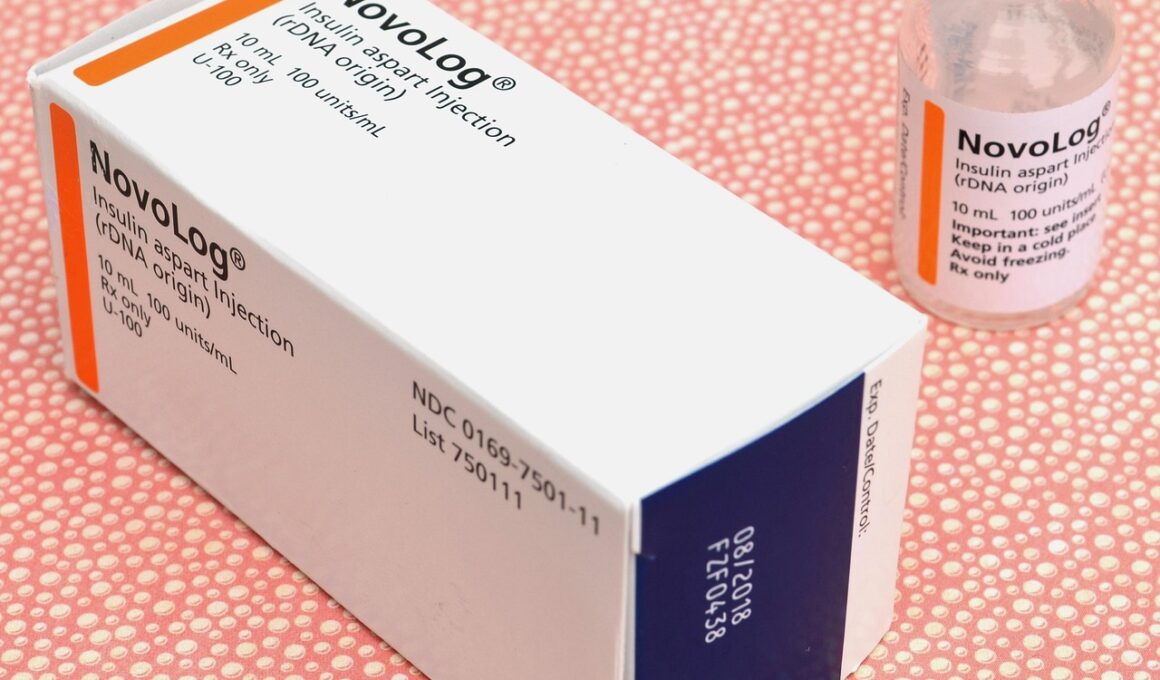
How to Safely Stop or Change Diabetes Medication
Managing diabetes often involves complex medication regimens, and if you’re considering stopping or changing your diabetes medication, it’s vital to do it safely. First, always consult with your healthcare provider before making any changes. Your doctor will have a comprehensive understanding of your personal health history, current medications, and potential implications of altering your treatment. They can provide tailored advice suited to your needs. Additionally, a gradual tapering off of medication is typically recommended rather than an abrupt stop, thus minimizing the risk of adverse effects. Observe how changes might influence your blood sugar levels and overall health. Keep a detailed log of these changes to discuss during follow-up visits. It is also helpful to have an action plan prepared for when you encounter high or low blood sugar levels during the transition. Communication with your healthcare team is crucial in this process. Employ felt support systems, such as family or diabetes support groups, to help navigate this journey. Remember, never self-medicate or modify dosages without professional guidance.
Nutrition plays a crucial role in the management of diabetes, especially in conjunction with medication. A well-balanced diet can have a positive impact on your blood sugar levels and overall health. Focus on incorporating a variety of whole foods into your meals, including leafy greens, lean proteins, whole grains, and healthy fats. Avoiding processed foods and sugary drinks is advisable, as they can cause spikes in your blood sugar. Keeping your carbohydrate intake consistent can also assist in managing diabetes effectively. Meal planning is a valuable tool, as it allows you to prepare balanced meals and snacks ahead of time. Consider working with a registered dietitian, who can help you create a personalized nutrition plan based on your specific requirements and preferences. They can also educate you on reading food labels and understanding portion sizes. Staying hydrated is essential, and water is the best option. Regular monitoring of your blood sugar will also guide you on how different foods affect your body. Monthly evaluations with a healthcare professional can ensure adjustments to your plan are made as needed. Always prioritize nutrient-dense choices for optimal health.
Potential Risks of Stopping Medication
Stopping diabetes medication without guidance can lead to serious health risks. When diabetes medications are stopped abruptly, blood sugar levels can spike dangerously high. This condition called hyperglycemia can result in symptoms like frequent urination, increased thirst, fatigue, and blurred vision. Long-term complications can arise if high blood sugar levels persist, including kidney damage, nerve damage, and cardiovascular issues. Another concern is the risk of diabetic ketoacidosis, especially for type 1 diabetes patients, which can be life-threatening if not treated promptly. Additionally, certain medications have withdrawal effects that can adversely impact your health if discontinued suddenly. To mitigate these risks, it’s essential to have a discussion with your healthcare provider about any symptoms you may experience. They may decide to adjust your medication or recommend alternative treatments based on your evolving needs. Monitoring your blood sugar closely during any transition is crucial for your safety. It’s vital to maintain open lines of communication with your healthcare team throughout this process to ensure a safe and effective management strategy.
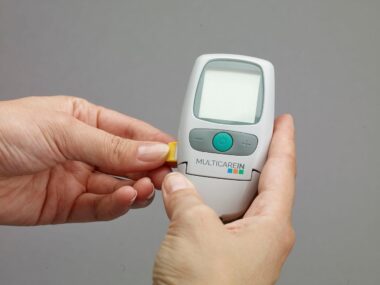
Understanding your body’s response to changes in medication is key to successful diabetes management. Regularly monitoring your blood sugar levels allows you to see how modifications in your treatment affect your glucose control. Utilizing a glucose meter or continuous glucose monitor can provide real-time data. This information can empower you to make informed decisions regarding your health. Documenting any noteworthy patterns in your blood sugar can be helpful for your healthcare provider during consultations. Be mindful of how your body feels; fatigue, hunger, and mood changes can be indicators of your body’s adjustment to a new regimen. Nutrition and lifestyle factors also play critical roles here. For example, changes in diet or exercise can significantly influence blood sugar levels. Establishing a routine that incorporates balanced meals and consistent physical activity can enhance overall management. Moreover, consider joining diabetes education programs or support groups, which can provide additional insights and community support. Your treatment should be personalized, and alterations should take into account your lifestyle and preferences to achieve sustainable results.
Alternative Treatment Options
There are various alternative treatment options for diabetes management that you can explore in conjunction with medication adjustments. For instance, incorporating more physical activity into your daily routine can improve insulin sensitivity, thus helping regulate blood sugar levels. Activities like walking, swimming, or yoga are excellent ways to stay active, increase fitness levels, and reduce stress. Mindfulness practices, such as meditation or deep-breathing exercises, can also help manage stress, which can otherwise lead to fluctuations in blood sugar levels. Additionally, some patients may benefit from nutritional supplements, like chromium or alpha-lipoic acid, but always consult your healthcare provider before adding these to your regimen. Another alternative is considering the use of insulin pumps or continuous glucose monitors, which can provide more flexibility and control over your condition. Acupuncture and certain herbal supplements are also explored by some individuals, but research evidence on their effectiveness is still emerging. Thoroughly discuss these alternatives with your healthcare provider to ensure they align with your overall treatment strategy and safety.
Support from family and friends plays an invaluable role in your journey of stopping or changing diabetes medication. Discuss your plans with those close to you, so they can offer encouragement and potentially help manage any stress related to this process. Often, loved ones can provide insights or reminders that assist in adhering to your medical plan, including medication schedules and dietary changes. Finding a diabetes support group can connect you with others facing similar challenges, offering a platform for sharing experiences, tips, and encouragement. Many local and online communities are available, providing a sense of belonging and understanding that is vital during transitions. Furthermore, social support can help reinforce the importance of maintaining healthy habits, staying active, and committing to regular check-ups. Don’t hesitate to lean on your community; whether that be in-person companions or online forums. These supportive interactions can significantly benefit your emotional and mental health throughout your journey. Collaborating with healthcare providers and utilizing a robust support network can encourage positive outcomes. Remember, you are not alone in this experience.
Follow-Up and Monitoring
After making changes to your diabetes medication, regular follow-up appointments with your healthcare provider are crucial. These appointments provide an opportunity to assess your progress and make any necessary adjustments to your treatment plan. Blood tests, such as HbA1c, are typically conducted to evaluate your average blood glucose levels over the past few months. This helps determine whether the changes to your medication are effective. Consistent monitoring can help catch any complications early on, ensuring prompt intervention. Your healthcare team can also help manage any side effects that may arise from new medications or dietary changes. Ensuring accessibility to healthcare providers after medication changes is vital for success. Keeping your medical records updated and sharing any new symptoms during appointments is equally important. Always express any concerns with your treatment to your provider. Collaborating closely with your team helps create a personalized and adaptable diabetes management plan that evolves with your needs. This ongoing process is essential for maintaining optimal health and quality of life as you navigate the changes in your diabetes management.
Achieving balance while managing diabetes requires a multifaceted approach. Ensuring that medication changes are made carefully and attended to with a continuous evaluation of your blood sugar levels is essential. Equally important is the integration of nutrition, exercise, and emotional support. Making gradual changes with the guidance of your healthcare team, along with remaining proactive in monitoring your health, ensures safety. Cultivating healthy habits not only helps reduce risks but also fosters a supportive environment conducive to better health outcomes. Utilize tools such as calorie tracking, blood sugar logs, and meal preparation strategies. Stay informed about new treatment options and strategies that promote successful management of diabetes. Engage in ongoing discussions with healthcare professionals about your needs and any changes to your regimen. Remember, every individual’s diabetes management plan should be unique and tailored to personal preferences and lifestyles. Combining all these elements aids in controlling your condition effectively while aligning with your long-term health goals. Success in managing diabetes is achievable when one focuses on a holistic and committed approach in partnership with their healthcare team.