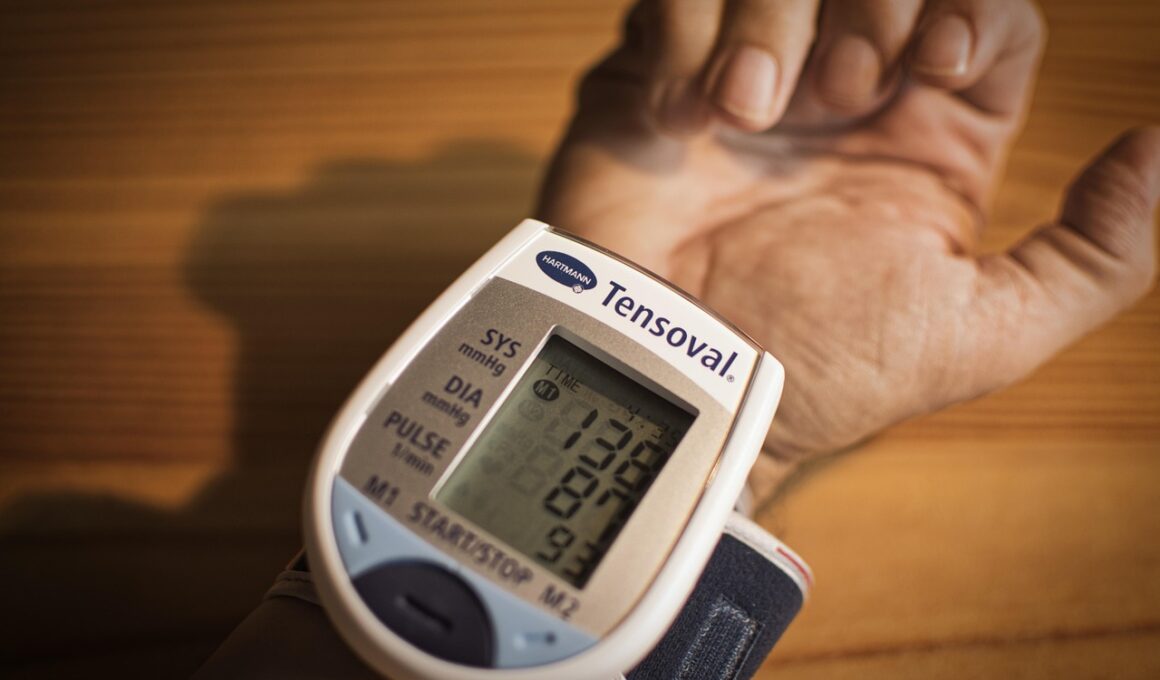
Fasting’s Impact on Blood Pressure Variability: What Studies Reveal
Fasting, traditionally associated with spiritual and health practices, has attracted scientific attention regarding its effects on various health parameters, especially blood pressure (BP). Research indicates that fasting can lead to significant changes in blood pressure variability (BPV). Blood pressure variability refers to the fluctuations in blood pressure readings within different times of the day. Studies have shown that intermittent fasting can decrease BP and stabilize BPV, which is crucial as high variability is linked to cardiovascular events. For individuals prone to hypertension, the relationship between fasting and BP becomes particularly relevant. Furthermore, fasting can contribute to weight loss, leading to improved overall cardiovascular health. More studies are needed, though, to establish a comprehensive understanding of how various fasting regimens affect blood pressure over the long term. Very few individuals are aware of fasting’s comprehensive benefits on blood pressure levels and variability. Individuals, particularly those with hypertension, should consult healthcare professionals before starting any fasting regime to ensure safe applicability and maximum benefits. This area of research can unveil innovative strategies for regulating blood pressure through dietary methods, such as fasting.
Several studies emphasize the favorable effects of fasting on blood pressure control. A study published in the American Journal of Hypertension demonstrated that participants engaging in intermittent fasting experienced a notable reduction in both systolic and diastolic blood pressure. Moreover, this reduction in BP appears to correlate with reduced body weight, decreased insulin resistance, and lower levels of inflammation. Another significant point is that fasting helps in resetting the body’s metabolic processes, which may lead to better regulation of BP. The impact of calorie restriction imposed by fasting is pivotal in producing these physiological changes. Participants reported improvements not only in their BP but also in other markers of cardiovascular health. Notably, fasting may also enhance the elasticity of blood vessels, which is vital for maintaining healthy blood pressure levels. With scientific evidence supporting these claims, it becomes crucial for healthcare providers to consider fasting as a potential therapeutic strategy for managing hypertension. Ultimately, understanding the multi-faceted benefits of fasting could guide individuals towards healthier lifestyles and dietary choices, benefiting both BP and overall wellbeing.
In addition to traditional styles of fasting, various modern intermittent fasting methods have gained popularity, such as the 5:2 and 16/8 approaches. These methods may further assist in moderating blood pressure levels without requiring drastic lifestyle changes. While the 5:2 method entails significantly decreasing caloric intake for two non-consecutive days each week, the 16/8 method restricts eating to an 8-hour window daily. Research suggests that adopting either approach can effectively impact blood pressure levels, improving not only BP itself but also enhancing metabolic flexibility and cardiovascular health. Participants have noted how these methods contribute to better weight management and decreased appetite, which are beneficial for long-term health. As fasting methods often integrate into daily routines comparatively easily, they provide an excellent starting point for those looking to engage in healthier eating patterns and lifestyle modifications. More clinical trials are needed to explore the mechanisms behind these effects in varied populations. By better understanding how different fasting styles impact BP, healthcare professionals can tailor recommendations that align with patient preferences and achieve favorable health outcomes.
Mechanisms Behind Fasting and Blood Pressure
Several mechanisms influence how fasting impacts blood pressure variability. First, fasting serves to improve insulin sensitivity, significantly decreasing levels of insulin in circulation. Elevated insulin levels can contribute to higher blood pressure and vascular resistance. Moreover, fasting induces autophagy, which is the body’s maintenance program, promoting cellular repair and reducing oxidative stress. This reduction in oxidative stress is essential for maintaining vascular health and normalizing blood pressure levels. Another crucial mechanism involves hormonal regulation; fasting influences certain hormones, including norepinephrine and cortisol, both of which impact vascular tone and blood pressure. The decrease in sympathetic nervous system activity during fasting may lead to overall lower blood pressure. Furthermore, studies indicate that fasting can influence the renin-angiotensin system, a hormone system that regulates blood pressure and fluid balance. All these interconnected mechanisms create a significant cumulative effect on blood pressure and its variability. Understanding these processes is vital for creating focused dietary strategies intended to support heart health and manage blood pressure effectively. Fasting shows promise as a non-pharmacological method for improving cardiovascular risk and could reshape treatment paradigms for hypertension.
Nevertheless, fasting may not be suitable for everyone, particularly individuals with pre-existing health conditions. For some populations, such as those with diabetes or specific metabolic disorders, the impact of fasting on blood pressure might require careful monitoring. These individuals may experience changes in medication requirements based on weight fluctuations or blood sugar levels during fasting periods. It is essential for healthcare professionals to provide personalized guidance to ensure that fasting is safe and effective for these patients. Additionally, it is equally important to consider the psychological aspects of fasting. Some individuals may struggle with the mental challenges associated with prolonged periods without food, potentially leading to binge eating. Addressing these concerns is vital in establishing a successful fasting practice. Fasting’s effect on blood pressure variability certainly carries promise, but balancing its advantages with potential risks is crucial. Encouraging patients to adopt a gradual and informed approach can contribute to positive health outcomes. Overall, the collaboration between healthcare providers and patients regarding fasting can lead to tailored strategies that effectively manage blood pressure and enhance overall wellbeing.
Future Research Directions
Future research is imperative to elucidate the nuanced relationship between various fasting regimens and blood pressure variability comprehensively. There remains significant variability among individual responses to fasting, indicating that personalized approaches should be taken. Extended clinical trials will enable researchers to assess the long-term effects of different fasting methods on not just blood pressure, but overall cardiovascular health. Beyond blood pressure itself, investigations should also include the broader impact of fasting on heart rate variability, endothelial function, and overall cardiovascular resilience. Understanding these correlations will provide deeper insights into how dietary interventions like fasting contribute to heart health. Moreover, studies should focus on analyzing the effects of fasting among diverse populations, including differing age groups, genders, and pre-existing health conditions. Furthermore, the potential for fasting to act as an adjunct therapy for pharmacological treatments in hypertensive patients remains an intriguing area for future exploration. Overall, ongoing interdisciplinary collaboration between nutritionists, healthcare providers, and researchers will propel advancements in the field. Fasting, in this context, stands to reshape public health initiatives aimed at promoting cardiovascular health and preventing hypertension.
In conclusion, the intersection of fasting and blood pressure variability highlights an exciting avenue of research with significant implications for public health. Studies strongly indicate that fasting, including various regimens, can effectively modulate blood pressure levels and contribute to better cardiovascular outcomes. As our understanding of fasting deepens, its role in managing hypertension and improving overall health emerges as increasingly clear. Patients and healthcare providers need to engage in open dialogues about the feasibility and safety of adopting fasting practices. Educational materials should be widely disseminated to elevate public awareness about the potential benefits of fasting on blood pressure and its variability. Ultimately, individuals seeking to implement fasting as a lifestyle change must recognize its profound effects on health and consider incorporating these practices into their routines responsibly. Hence, future research must continue to explore fasting’s multifactorial benefits, paving the way for innovative dietary strategies to combat a global hypertension epidemic. By harnessing the potential of fasting, we may uncover effective approaches to enhance individual health and improve community well-being through informed dietary practices.