The Relationship Between Obesity and Gut Microbiome Disorders
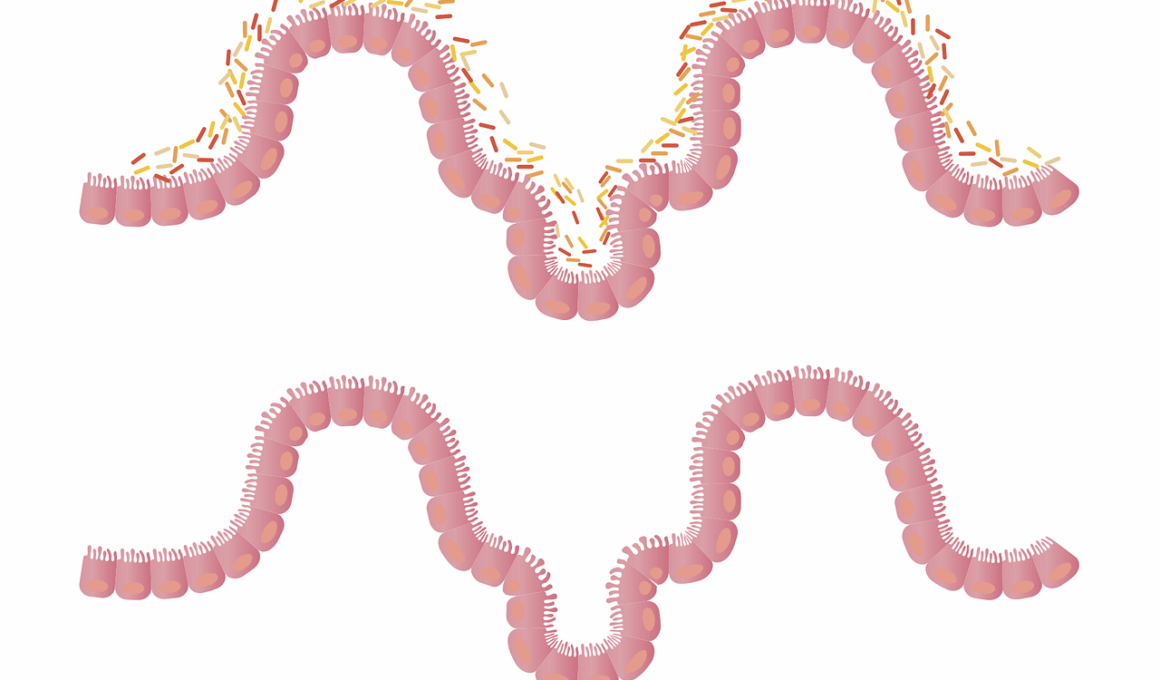
The intricate relationship between obesity and gut microbiome disorders is a growing area of research. Recent studies suggest that the gut microbiome’s composition significantly influences an individual’s body weight and metabolic health. A diverse gut microbiome is linked to better nutrient absorption and fat storage regulation. Conversely, an imbalance, known as dysbiosis, may trigger inflammatory responses that contribute to obesity. Factors contributing to dysbiosis include poor diet, lack of exercise, and antibiotic use, which can drastically alter microbial populations. Specifically, reductions in beneficial bacteria like Faecalibacterium and Akkermansia are often observed in obese individuals. This suggests a potential pathway through which gut health can influence weight. Obesity reduces microbial diversity, leading to higher levels of pathogenic bacteria. This imbalance not only affects metabolism but may also increase the risk of other metabolic diseases, such as diabetes. Understanding these mechanisms can help develop strategies to modify the gut microbiome to promote weight loss and metabolic health, potentially altering treatment approaches for obesity globally. Further research is essential to explore these connections comprehensively.
Gut Microbiome’s Role in Metabolism
The gut microbiome plays a pivotal role in metabolic processes, including digestion and energy extraction from foods we consume. Studies indicate that the microbiome helps digest complex carbohydrates, producing short-chain fatty acids (SCFAs) that regulate appetite and influence overall metabolism. Obese individuals often display lower levels of SCFAs, correlating with increased hunger and fat storage. In contrast, lean individuals tend to have thicker gut walls rich in beneficial microbiota that contribute to a healthy energy metabolism. The microbial action also affects the hormone levels responsible for hunger and satiety, such as ghrelin and leptin. An imbalance in gut microbiota may disrupt hormonal signaling, promoting overeating behaviors, hence contributing to obesity. Additionally, the microbiome can affect insulin sensitivity, leading to complications like type 2 diabetes. Increasing dietary fiber intake is one way to enhance the diversity of gut bacteria and improve metabolic health. Encouragingly, positive dietary strategies that include fermented foods can restore a healthy microbiome balance, thus improving metabolic regulation, supporting sustainable weight loss programs, and enhancing overall wellness.
Gut microbiome disorders have shown a significant correlation with inflammation, particularly concerning obesity. Chronic low-grade inflammation is characteristic of obesity and plays a crucial role in the development of related disorders. Gut bacteria have a profound impact on the immune system, with dysbiosis linked to increased production of inflammatory cytokines. Such cytokines may cause insulin resistance and lead to metabolic syndrome, posing severe health risks. Therefore, maintaining gut health is essential for preventing obesity and its complications. Anti-inflammatory foods, such as leafy greens, probiotics, and omega-3 fatty acids, can positively influence gut health and the immune response. Conversely, a diet high in sugar and saturated fats can worsen inflammation, using dysbiosis as a catalyst for further metabolic issues. Among the notable metabolic diseases, non-alcoholic fatty liver disease (NAFLD) has emerged as a severe consequence of obesity, related to gut health issues. Addressing the interplay between diet, inflammation, and microbiome health could represent a key strategy in combating rising obesity rates worldwide. Therefore, lifestyle interventions focusing on gut health may offer promising avenues for effective weight management.
Potential Therapeutics Targeting Gut Microbiome
Various approaches to therapeutically target and restore a healthy gut microbiome are being explored to combat obesity. Probiotics, prebiotics, and dietary modifications represent three primary methods of promoting beneficial bacteria. Probiotics involve the direct introduction of live beneficial microorganisms, while prebiotics emphasize feeding existing healthy bacteria a diet rich in fiber and resistant starches. Studies indicate that incorporating these may significantly improve microbiome health and metabolic outcomes in obese patients. Fecal microbiota transplantation (FMT) is an innovative technique that aims to replace harmful bacteria with health-promoting strains, leading to promising results in clinical trials. This procedure restores a balanced microbiome, resulting in weight reduction and improved metabolic indicators. However, more research is necessary to determine the long-term efficacy and safety of FMT as a treatment option. Moreover, personalized medicine approaches that consider an individual’s unique microbiome composition and genetic predisposition could lead to tailored interventions. Ultimately, understanding these therapeutic avenues will hopefully enable healthcare providers to mitigate obesity and its related disorders in diverse populations effectively.
Nutritional strategies also play a crucial role in restoring gut microbiome health. Consuming a balanced diet rich in fiber, vitamins, and minerals can enhance microbial diversity. A diet incorporating fruits, vegetables, legumes, whole grains, and fermented foods ensures a steady supply of prebiotics and probiotics, nourishing beneficial gut bacteria. Furthermore, reducing processed foods, sugary beverages, and unhealthy fats can limit the proliferation of harmful bacteria that may contribute to obesity. Hydration is another essential factor; adequate water intake supports digestive health and facilitates the beneficial functions of the microbiome. Beyond diet, regular physical activity significantly impacts gut health by promoting microbial diversity and enhancing metabolic processes. Different forms of exercise have been shown to cultivate a favorable microbiota, contributing to weight management. Interventions combining strategic dietary alterations with consistent exercise may thus provide a comprehensive approach to support gut health and tackle obesity. As awareness of the gut-brain connection grows, fostering optimal gut health could be integral to achieving a healthier body weight and improved well-being overall.
The Future of Gut Microbiome Research
Looking ahead, the field of gut microbiome research is poised for exciting advancements that can reshape our understanding of obesity and related disorders. The exploration of microbiome-host interactions continues to unveil novel pathways for therapeutic interventions. Applying next-generation sequencing technologies enables researchers to profile complex microbial communities in unprecedented detail. This ability enhances the identification of specific bacterium associated with obesity and metabolism. Innovations in metagenomics and metabolomics allow scientists to dissect the metabolic activities of microbial populations, fostering targeted treatments for dysbiosis. Longitudinal studies tracking microbiome changes in relation to dietary patterns and lifestyle choices will offer insights into effective prevention and management strategies. Furthermore, personalized microbiome-based therapies could emerge as a standard practice for obesity treatment. As research expands, public awareness will also play a vital role in promoting gut health. Education initiatives need to highlight the importance of maintaining a healthy gut microbiome through informed lifestyle choices. Engaging communities in the conversation about gut health can foster collective action towards preventing obesity and enhancing overall health on a broader scale.
To conclude, the relationship between obesity and gut microbiome disorders is complex yet crucial in understanding metabolic health. Ongoing research is demanding increased attention to the role of gut health in weight management, revealing potential avenues for innovative interventions. By focusing on restoring gut microbial balance through dietary strategies, physical activity, and targeted therapies, significant progress can be achieved in combating obesity. The implications of gut microbiome research extend beyond obesity, influencing diverse health outcomes. Establishing a direct connection between gut health and obesity highlights the need for integrated approaches that prioritize holistic and preventive health measures. Policymakers, healthcare providers, and individuals alike should be motivated to consider gut health as a cornerstone of obesity management strategies. Implementing community health programs targeting dietary education and lifestyle changes can lead to significant positive changes in public health. As understanding deepens, the future may reveal more refined methods to harness the gut microbiome’s potential, fostering healthier populations and reducing the burden of obesity and related disorders worldwide. The continuity of gut microbiome research is vital for an optimized approach toward health promotion and disease prevention.
Conclusion
The relationship between obesity and gut microbiome disorders underscores the necessity for a multifaceted approach in modern health strategies. Recognizing the role of gut health in overall metabolic regulation provides a new lens through which to view obesity and its related challenges. Promoting awareness of gut microbiome health can empower individuals to make informed dietary choices that support their well-being. As research progresses, the potentials for targeted interventions continue to expand, allowing for personalized approaches that cater specifically to individual needs. Public health initiatives aimed at reducing obesity must now integrate the importance of gut microbiome health into their frameworks. By advocating for healthier food environments and lifestyles, significant strides in combating the obesity epidemic can be made. We are only beginning to scratch the surface of what the gut microbiome has to offer, and its role will undoubtedly grow in both clinical settings and everyday health discussions. Ultimately, a healthier gut microbiome could be a pivotal step in reaching healthy weight status and preventing chronic diseases, paving the way for enhanced quality of life and longevity.