How Gut Microbiome Influences Autoimmune Conditions
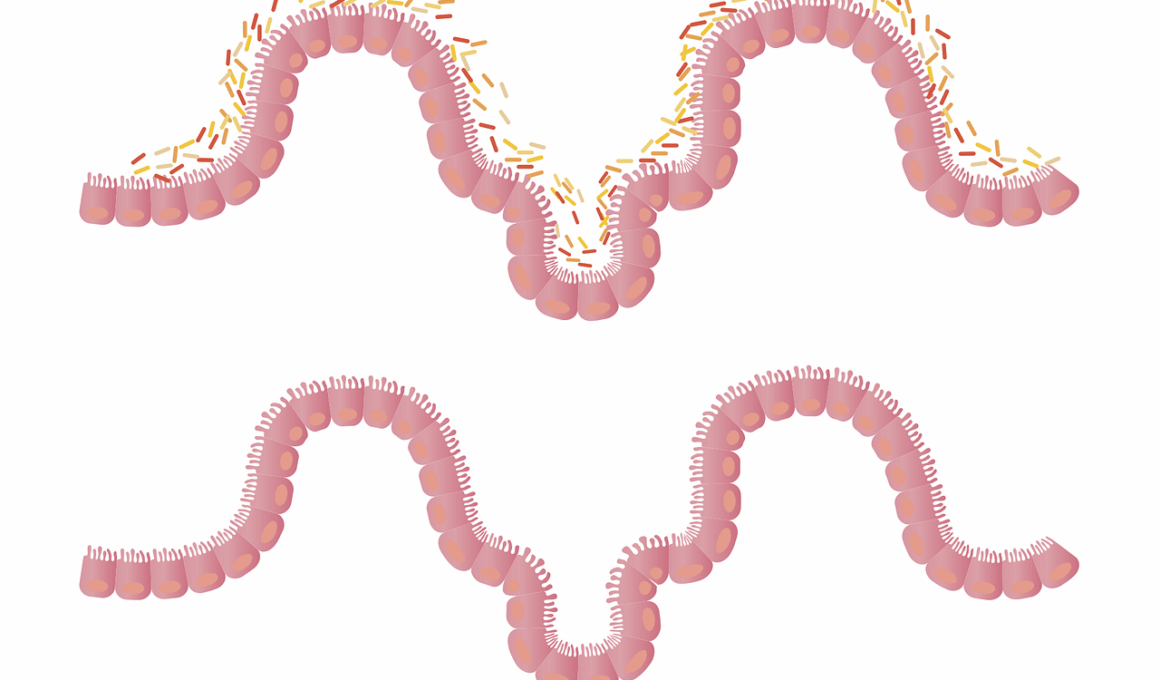
The relationship between gut health and autoimmune diseases has gained attention over recent years. Scientific studies reveal that the gut microbiome plays an essential role in regulating immune responses. A healthy gut consists of a diverse range of bacteria. This diversity is crucial for preventing inflammation, which can trigger autoimmune conditions such as rheumatoid arthritis and lupus. When the gut microbiome is disrupted, it may lead to an imbalance in gut flora. This imbalance can increase intestinal permeability, often referred to as ‘leaky gut.’ Consequently, bacteria and toxins can enter the bloodstream. These substances can prompt the immune system to become hyperactive, potentially leading to autoimmune reactions. Many researchers are focusing on how restoring microbiome balance may provide therapeutic benefits. Probiotics and prebiotics are commonly suggested to support gut health. It is essential to consider dietary habits that promote microbiome diversity. Incorporating fermented foods, fiber-rich vegetables, and whole grains can enhance gut health. Each of these elements contributes positively to the maintenance of an optimal gut microbiome. This discussion opens several avenues for further research into managing autoimmune diseases through gut interventions.
The Role of Diet in Gut Microbiome Health
A balanced diet significantly influences gut microbiome health. Dietary choices directly affect the diversity and composition of gut bacteria. Foods rich in fiber, such as fruits, vegetables, and legumes, serve as fuel for healthy bacteria. This nourishing effect plays a crucial role in gut health. The consumption of fermented foods, such as yogurt and kimchi, introduces beneficial bacteria, which can further support microbiome diversity. Furthermore, processed foods high in sugar and unhealthy fats may negatively impact gut flora. Research indicates that Western diets, characterized by high sugar and fat content, are linked to reduced microbial diversity. This decline can lead to inflammation and contribute to the development of autoimmune diseases. Additionally, specific diets, like the Mediterranean or plant-based diets, found to enhance gut health, emphasize fruits, vegetables, whole grains, and healthy fats. Implementing such dietary patterns may improve not only gut health but also overall well-being. Staying hydrated is also critical for maintaining a well-functioning gut. Therefore, being mindful of food choices is vital in fostering a healthy gut microbiome and mitigating autoimmune conditions in susceptible individuals.
Understanding the Connection Between Inflammation and Gut Health Chronic inflammation is a central factor in many autoimmune diseases. The gut microbiome significantly influences inflammation levels. Dysbiosis, or an imbalance in gut bacteria, can result in increased production of pro-inflammatory cytokines. This overactive immune response can potentially lead to the manifestation of autoimmune disorders. Understanding this connection clarifies the potential of microbiome-related therapies for managing inflammation. When gut bacteria are balanced, they can help regulate immune activity, thereby reducing inflammation. For example, certain strains of probiotics have shown promise in decreasing inflammatory markers in clinical studies. By decreasing inflammation, these beneficial bacteria may alleviate symptoms associated with autoimmune diseases. Lifestyle factors also contribute to inflammation in the body. Stress management, sleep quality, and physical activity play roles in maintaining a healthy immune response. Engaging in mindfulness practices, prioritizing adequate sleep, and maintaining regular exercise can help support a balanced immune system. It is essential to explore these aspects further to discover effective strategies for individuals affected by autoimmune disorders. Overall, integrating gut health into inflammation management can lead to comprehensive therapeutic approaches.
Exploring the Gut-Brain Connection
The gut-brain connection is an emerging field of study that highlights the interplay between gut health and mental well-being. Research shows that the gut microbiome influences not only physical health but also emotional health. This relationship can have implications for individuals with autoimmune conditions, many of which are associated with mental health challenges. The gut produces various neurotransmitters that affect mood and cognition, including serotonin. A complicated network of signals between the gut and brain affects emotional states. Imbalances in gut bacteria may lead to anxiety and depression, particularly among individuals with autoimmune diseases. Simultaneously, psychological stress can negatively impact gut health. Stress can alter gut permeability and microbiome composition, creating a bidirectional relationship. Supportive therapies for individuals with autoimmune disorders could include addressing mental health as part of treatment. Strategies such as mindfulness practices, meditation, and stress-reducing activities may provide significant benefits. Integrating psychological and nutritional support may improve the overall quality of life for those experiencing autoimmune conditions. Future research will continue to unveil the complex interactions within the gut-brain axis and their relation to autoimmune diseases.
Role of Prebiotics and Probiotics in Autoimmune Management Prebiotics and probiotics have become popular for promoting gut health and may play crucial roles in managing autoimmune conditions. Prebiotics are types of fiber that feed beneficial gut bacteria, while probiotics are live microorganisms that enhance gut flora. A balanced intake of these elements can vary in improving immune function. Clinical studies indicate that specific probiotic strains can reduce inflammation and modulate immune responses. Moreover, some evidence suggests that probiotics can alleviate symptoms of certain autoimmune diseases. On the other hand, prebiotics can serve as a long-term strategy to maintain microbiome balance. Foods high in prebiotics include garlic, onions, and asparagus. Each serves as nourishment for healthy gut bacteria, fostering their growth. The combined intake of prebiotics and probiotics is often referred to as synbiotics. Dietary supplements containing both have shown promise in clinical trials. Incorporating synbiotics into nutritional plans could optimize gut conditions. This approach may ultimately contribute to better management of autoimmune conditions. It is essential to consult healthcare professionals before initiating any new regimens to ensure their relevance and effectiveness.
The Future of Gut Health Research
As research in gut health evolves, it reveals new pathways for understanding autoimmune diseases. The field is rife with potential for developing novel therapeutic approaches. Investigating the gut microbiome’s complexity provides insights into how specific bacterial strains may influence immune regulation. Future studies may identify biomarkers linked to diverse microbiome health. Such discoveries could enable personalized treatments aimed at restoring microbiome balance for individuals with autoimmune disorders. Beyond diet and supplementation, lifestyle factors will remain crucial in future research. Understanding the influence of exercise, sleep, and stress management on gut health could lead to comprehensive treatment plans. Identifying interactions between various dietary patterns and gut microbiomes may yield personalized nutrition recommendations. Innovations in technology also offer insights into assessing gut health. Metagenomic sequencing will provide detailed information about microbiome composition. Integrating these technologies can help connect specific gut bacteria to autoimmune reactions and diseases. Ultimately, a multidisciplinary approach that considers genetics, environment, diet, and lifestyle will be essential for advancing gut health research. Future developments could pave the way for targeted therapies aimed at managing autoimmune diseases and promoting overall health.
Conclusion The connection between gut health and autoimmune diseases illustrates the complexity of our body’s systems. The gut microbiome is a vital player in our immune responses and overall health. Maintaining gut health through good dietary practices, mindful lifestyle choices, and, when necessary, the use of prebiotics and probiotics can have significant effects. As the field continues to develop, promising new therapies may emerge, tailored to individual needs for managing autoimmune conditions. Continued research will explore the intricate dynamics of the gut microbiome and its implications for health. The potential for integrating gut health with conventional medical treatments presents exciting avenues for patients. Holistic approaches that encompass diet, lifestyle, and mental health factors are poised to yield the most significant benefits in autoimmune disease management. Staying informed and proactive about gut health will empower individuals to take charge of their health journeys. Improved understanding will continue to enhance the relationship between gut microbiomes and the body. This field’s exploration is just the beginning, encouraging proactive interventions and increased resilience against autoimmune diseases.
Autoimmune diseases engage the body’s defense system inappropriately, targeting healthy cells. Gut health is pivotal in understanding these complex conditions. The gut microbiome contributes greatly to the regulation of immune functions. A healthy microbiome aids in maintaining a balanced immune response, preventing unnecessary attacks on the body. Disturbance in gut flora can exacerbate inflammation, often triggering autoimmune responses. Researchers are focusing on various aspects to comprehend how gut health impacts these diseases. Some studies examine specific bacterial populations associated with autoimmune conditions. Others consider how gut metabolites affect immune signaling pathways. Diet remains particularly critical in shaping gut health. Eating anti-inflammatory foods could provide protective effects. Foods rich in omega-3 fatty acids, for example, can counteract inflammation. Engaging in these dietary strategies while promoting diverse gut bacteria offers hope for managing autoimmune diseases. Taking steps to restore and maintain gut balance could be an essential part of restoring overall health. Future advancements in gut health research will continue to shed light on these intricate connections. As public awareness grows, so does the call for further exploration of the gut’s role.