Understanding Fasting’s Effect on Digestive Health Biomarkers
Fasting, an age-old practice, has drawn considerable attention due to its potential benefits for digestive health. Scientific research has started to confirm its effects on various digestive health biomarkers, which are essential indicators of overall gastrointestinal function. Various studies suggest that intermittent fasting and prolonged fasting can enhance gut health by promoting beneficial changes in the gut microbial composition. The gut microbiome plays an essential role in digestion, metabolism, and immune function, so any improvement can have widespread implications. Key benefits include improved insulin sensitivity, lower levels of inflammation, and enhanced stool consistency. These changes can help alleviate common digestive issues such as bloating, constipation, or irritable bowel syndrome. Furthermore, fasting may promote autophagy, a process that helps in cellular repair within the digestive system. Through this mechanism, the body can effectively eliminate damaged cells, leading to overall improved gut health. Individuals interested in fasting therapies should consult healthcare professionals to tailor specific fasting protocols based on personal needs and health conditions. The evidence supporting fasting continues to grow, making this ancient practice increasingly recognized for its modern health benefits.
Impact on Inflammation and Gut Microbiota
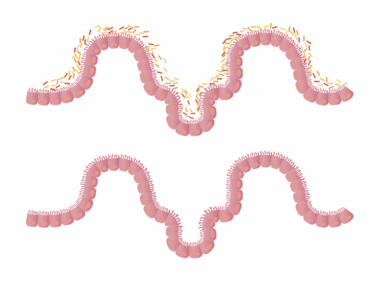
One of the most notable effects of fasting is its ability to reduce inflammation in the body, particularly within the gastrointestinal tract. Inflammation is often a precursor to various digestive disorders and conditions. Fasting has been shown to lower the production of inflammatory cytokines, leading to a more balanced immune response in the gut. Furthermore, fasting is believed to enrich beneficial gut microbiota, which is crucial for digestive health. During fasting periods, beneficial bacteria flourish, fostering an environment conducive to enhanced digestion and nutrient absorption. Another important aspect involves the release of short-chain fatty acids, which have anti-inflammatory properties and provide energy to the intestinal cells. Through these interactions, fasting not only improves bodily inflammation but also increases the diversity of gut bacteria, contributing to greater resilience against gastrointestinal diseases. Regular fasting practices may potentially enhance the microbiome landscape and lower the risk of chronic conditions. These benefits collectively signify an emerging field of study focusing on fasting as a holistic approach to promote digestive health effectively.
Fasting can significantly improve digestive health by facilitating better enzymatic activity in the gastrointestinal tract. Enzymes play a pivotal role in breaking down nutrients, and their efficacy is influenced by various factors, including dietary habits. During fasting, the digestive system gets a much-needed rest, allowing for the regeneration of gut lining and improving enzyme secretion when food is eventually consumed. Digestive enzymes aid in breaking down proteins, carbohydrates, and fats, leading to enhanced nutrient absorption. Additionally, the production of bile, essential for fat digestion, may become more efficient due to the improved function of the liver during fasting periods. This rest is critical, as many people experience overworked digestive systems due to constant food intake and poor dietary choices. Fasting thus serves not only as a dietary strategy but also as a health and wellness practice that allows the gut to rejuvenate. As digestive health becomes increasingly recognized as foundational to overall well-being, fasting may be an effective tool to foster optimal gastrointestinal function, improve nutrient availability, and minimize digestive discomfort.
Effects on Gut Hormones
A fascinating aspect of fasting is its influence on gut hormones, which regulate various digestive processes in the body. Hormones like ghrelin and leptin play critical roles in hunger signals and satiety but also affect digestion. Studies indicate that fasting can help balance these hormones, improving appetite control and digestive efficiency. For instance, fasting may lead to lower levels of ghrelin, often referred to as the hunger hormone, which can help curb unnecessary snacking and promote a healthier eating pattern. Additionally, fasting can enhance the secretion of hormones like glucagon-like peptide-1 (GLP-1), which aids in insulin secretion and slows gastric emptying, leading to better nutrient absorption. Better hormone regulation translates to improved digestive processes, allowing for smoother digestion and enhanced metabolic function. Overall, the relationship between fasting and gut hormones reveals that this ancient practice can play a crucial role in optimizing digestive health and managing weight. For individuals aiming for weight management or improved gut health, incorporating fasting into their lifestyle might prove beneficial.
The impact of fasting on digestive health extends beyond hormones and enzymes to include its effects on gastrointestinal motility. Gastrointestinal motility refers to the movements of the digestive tract that facilitate food movement and processing. Research has indicated that fasting may help regulate and improve these movements, which is particularly beneficial for individuals suffering from digestive disorders like constipation or irritable bowel syndrome. Improved motility ensures that food passes through the gut at a healthier pace, promoting thorough digestion and reducing discomfort. Additionally, fasting provides the body with time to repair any abnormalities in the gut lining that may be hindering proper motility. Effective gut motility contributes not only to better nutrient absorption but also to improved overall digestive comfort. Such benefits highlight the importance of timing in food intake and suggest that strategic fasting could enhance the efficiency of the digestive process. Understanding the mechanisms by which fasting influences gut motility can help promote digestive well-being and guide therapeutic fasting practices for health improvements.
Connection to Gut Health and Chronic Diseases
Fasting has become an increasingly valued approach in holistic health practices due to its promising connection to disease prevention. Chronic diseases like obesity, diabetes, and inflammatory bowel disease have been linked to poor gut health. Emerging evidence suggests that fasting can reduce the risk of these conditions by promoting better digestive health. It offers a preliminary reset for the system, facilitating processes that lower inflammation, optimize gut flora, and enhance overall gut functionality. Furthermore, by reducing insulin resistance, fasting plays a critical role in metabolic health, which is closely related to digestive diseases. Research shows that individuals who adopt a fasting regimen often report fewer gastrointestinal symptoms and a marked reduction in chronic disease risk markers. Understanding the correlations between fasting practices and chronic diseases can provide insights into effective preventive health strategies. By embracing fasting, individuals can take a proactive stance against disease while fostering a healthier digestive environment. This could pave the way for integrating fasting into medical and wellness frameworks for enhanced public health.
As research continues to unravel the complexities of fasting, it becomes clear that its effects on digestive health are both multifaceted and profound. Understanding how fasting impacts digestive health biomarkers is crucial for individuals seeking to optimize their gastrointestinal function. Fasting not only encourages physical changes in metabolism but also promotes mental clarity, emotional well-being, and a nutritious perspective towards food. Individuals embarking on a fasting journey should prioritize awareness of their unique digestive needs. Consulting a healthcare professional for guidance can help individuals identify appropriate fasting schedules, whether intermittent or prolonged. Awareness of physiological and psychological responses during fasting is paramount to maximize benefits without discomfort. Fasting can be effectively tailored to suit varied lifestyles and health objectives, making it accessible to those wanting to experience its advantages. As the body adapts to fasting rhythms, individuals may notice improvement in energy levels, digestive efficacy, and overall health. Promoting flexibility and sustainability in fasting protocols is critical for long-term success. Ultimately, the journey towards improved digestive health through fasting can empower individuals by fostering a deeper relationship with their bodies and enhancing overall quality of life.
Conclusion
The intersection of fasting and digestive health represents a promising frontier in health and wellness studies. Through understanding its effects on digestive health biomarkers, we can begin to appreciate how periodic fasting may contribute to promoting a healthier and more resilient gut. The evidence suggests that fasting can influence inflammation, gut microbiota, enzymatic activity, gut hormones, and overall motility. Such benefits have broad implications for preventing chronic diseases linked to poor digestive health. As more people seek natural and effective strategies for wellness, fasting may emerge as an indispensable tool for holistic health. However, it should always be approached with caution and guided by medical expertise to ensure safety and effectiveness. Educating individuals on fasting principles can help in achieving desired outcomes while minimizing adverse effects. Combine fasting with balanced nutrition and lifestyle practices for optimal results. Collectively, individuals can enhance not only their digestive health but also improve their emotional and physical well-being. Embracing the wisdom of fasting can pave the path towards a healthier future, marking it as an invaluable approach for digestive health optimization.