Interpreting ECG Results: What Patients Need to Know
An electrocardiogram (ECG) is a crucial diagnostic tool for assessing heart health. It graphically displays the electrical activity of the heart over time. Patients may receive an ECG for various reasons, including irregular heartbeats, chest pain, or preoperative evaluations. The results can reveal several conditions, such as arrhythmias and ischemic heart disease. Understanding these results is essential for patients, as it can lead to timely interventions. After an ECG, patients often receive a report summarizing findings and recommendations. These documents may include interpretations of rhythm patterns and heart rate. Knowing how to interpret these reports can empower patients to take charge of their heart health. Various resources, including online articles and healthcare provider discussions, can aid understanding. Patients are encouraged to ask their doctors questions about any unclear figures or terms in their reports. Moreover, obtaining a copy of the ECG can assist in tracking heart health over time. Overall, being informed about your ECG results is a critical step to enhancing heart health, leading to better communication with healthcare professionals and improved outcomes.
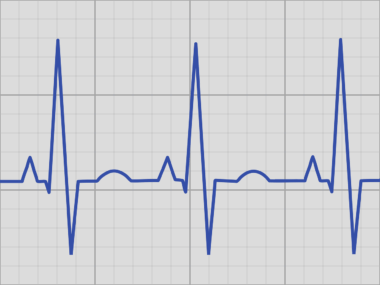
ECG printouts display waveforms that illustrate heartbeats. Analysis typically looks for identifiable waves, including P, QRS, and T waves. The P wave indicates atrial depolarization, while the QRS complex reflects ventricular depolarization. Finally, the T wave denotes ventricular repolarization. Document interpretation scrutinizes these waves for regularity, duration, and amplitude. For example, a prolonged QRS duration could signal a bundle branch block, while an odd T wave can suggest ischemia. Thus, knowing what each component signifies aids in understanding your cardiac condition. Additionally, sometimes ECGs are classified into different types, notably resting ECGs, stress tests, and Holter monitors. Each test serves a specific purpose in revealing how well your heart functions under various conditions. It is also vital to recognize that while an ECG is an excellent initial assessment tool, it might not capture all heart issues. Some conditions may require further testing, such as echocardiograms or blood tests. Patients should have ongoing dialogues with their healthcare providers about follow-up tests if any potential issues arise from the ECG results.
What to Expect During the ECG Procedure
Undergoing an ECG is a straightforward and non-invasive procedure. The healthcare provider will have you lie down and attach several electrodes to your chest, arms, and legs. These electrodes are small sticky patches that connect to the ECG machine. Patients may be asked to breathe normally, relax, and avoid moving during the test to ensure accurate readings. The entire process typically lasts about 10 minutes. After the electrodes are placed, the machine will record the electrical signals from the heart. Patients will hear the machine ticking or humming while it works. One common concern is skin irritation from the electrodes; however, it generally resolves quickly. An ECG is painless, and most patients feel comfortable throughout the procedure. Once completed, the healthcare provider will remove the electrodes, allowing patients to return to their daily activities immediately. It’s important to inform the provider of any medications taken, as these might affect the results. Post-procedure, you may discuss preliminary findings with your doctor during a follow-up appointment, ensuring you understand the implications for your heart health.
The interpretation of ECG findings often involves specialized healthcare professionals, such as cardiologists or trained technicians. These experts analyze the records for irregularities that might suggest underlying health conditions. For instance, arrhythmias can be identified by looking at the rhythm’s consistency and timing between beats. Any observed anomalies can lead to further exploration, such as lifestyle recommendations, medications, or additional testing. Patients should know that their unique medical history and risk factors play a crucial role in the ECG interpretation. Other tests can complement the ECG, such as echocardiograms, which provide imagery of the heart’s structure and function. This added data can help determine the best path forward in managing cardiac health. Understanding the collaborative nature of diagnosis emphasizes the need for open communication between patients and their healthcare teams. Asking about further recommendations based on ECG results is essential for effective health management. Ultimately, this integrated approach can significantly improve heart health outcomes. Moreover, many healthcare facilities provide educational resources to assist patients in comprehending their tests and treatments better.
Common Misconceptions About ECGs
Myths and misconceptions about ECGs can lead to misunderstandings regarding heart health. Many people mistakenly believe that an ECG can diagnose all heart conditions; however, it mainly assesses electrical activity. Some assume that only symptomatic individuals require ECGs, but routine screenings are also recommended for high-risk individuals. Furthermore, ECG results might not indicate an acute event, which can be discouraging for patients awaiting immediate answers. Understanding that ECGs play one part in the broader diagnostic process is crucial. Patients often wonder if they need to prepare differently for an ECG. In truth, most do not cause significant preparation, but avoiding heavy meals, caffeine, and exercise before testing can lead to clearer results. It is beneficial to recognize that these adjustments can help facilitate accurate readings. Patients are strongly encouraged to discuss any concerns or queries with their healthcare providers during consultations, as clarity can enhance understanding. Breaking down these misconceptions creates a more informed patient base, ultimately leading to better health choices and engagement with their healthcare teams regarding heart health.
Heart rate variability is another crucial factor assessed during an ECG. A normal heart’s rhythm shows variability, reflecting that the heart can adapt to different demands. Reduced variability can indicate an increased risk for cardiac events. This underscores the importance of a holistic approach when interpreting results from an ECG. Lifestyle factors, including exercise, stress, and nutrition, significantly influence heart rhythm. Doctors often recommend regular physical activity, as it can enhance cardiovascular health and improve heart rate variability. Nutrition plays a pivotal role in supporting heart health as well. Diets rich in lean proteins, whole grains, fruits, and vegetables benefit heart function. Moreover, stress management techniques can also improve outcomes related to heart health. Activities such as yoga or meditation can contribute to a healthier heart rhythm pattern. Patients should work with healthcare teams to develop personalized plans that incorporate these elements for better overall outcomes. Awareness of heart health encourages individuals to take proactive steps towards maintaining a well-functioning cardiovascular system. Regular follow-up consultations are vital to track improvements over time and adjust treatment plans as necessary.
Conclusion: Empowering Patients Through Knowledge
Understanding ECG results is empowering for patients, allowing them to take control of their cardiac health actively. Knowledge of the procedure, results interpretation, and the significance of follow-up care creates a foundation for informed discussions. Patients must feel comfortable asking questions and seeking clarification from healthcare providers, ensuring they grasp the implications of their results. Heart health is an ongoing journey that encompasses lifestyle choices and regular monitoring. By embracing educational resources, patients can better understand their situations and make informed choices. Building a partnership with healthcare providers enables individuals to tailor their approaches to health management effectively. This duo approach cultivates an environment where heart health can thrive. Ensuring that all necessary tests are performed and followed up is vital to long-term well-being. Ultimately, staying informed and engaged in one’s health can lead to enhanced outcomes and quality of life. Family support and peer relationships can also contribute significantly to motivation and adherence to health plans. This collaborative effort promotes transparency between patients and professionals, enhancing the overall healthcare experience and leading to healthier communities.
Patients are encouraged to share their experiences and success stories related to heart health and ECG testing. These narratives can foster a sense of community and support among those facing similar challenges. Emphasizing the importance of mental well-being alongside physical health underscores the comprehensive nature of cardiac care. Discussions about cardiovascular health can promote greater awareness within communities about the significance of routine screenings and risk factor modifications. Therefore, armed with knowledge and support networks, patients can engage in conversations that promote heart health among peers. Engaging in community programs, educational seminars, and support groups focused on heart health can significantly improve awareness as well. Having accessible channels for sharing knowledge creates an environment where individuals can learn from one another. Awareness campaigns often educate the public on the warning signs of heart issues, encouraging proactive health measures. Engaging with online resources like forums and webinars also expands knowledge. In conclusion, through community efforts and shared experiences, patients can further promote awareness, drive dialogue about heart health, and help others gain the insights needed for healthier lives.