Understanding the Impact of Antibiotics on Mental Health via Gut Flora
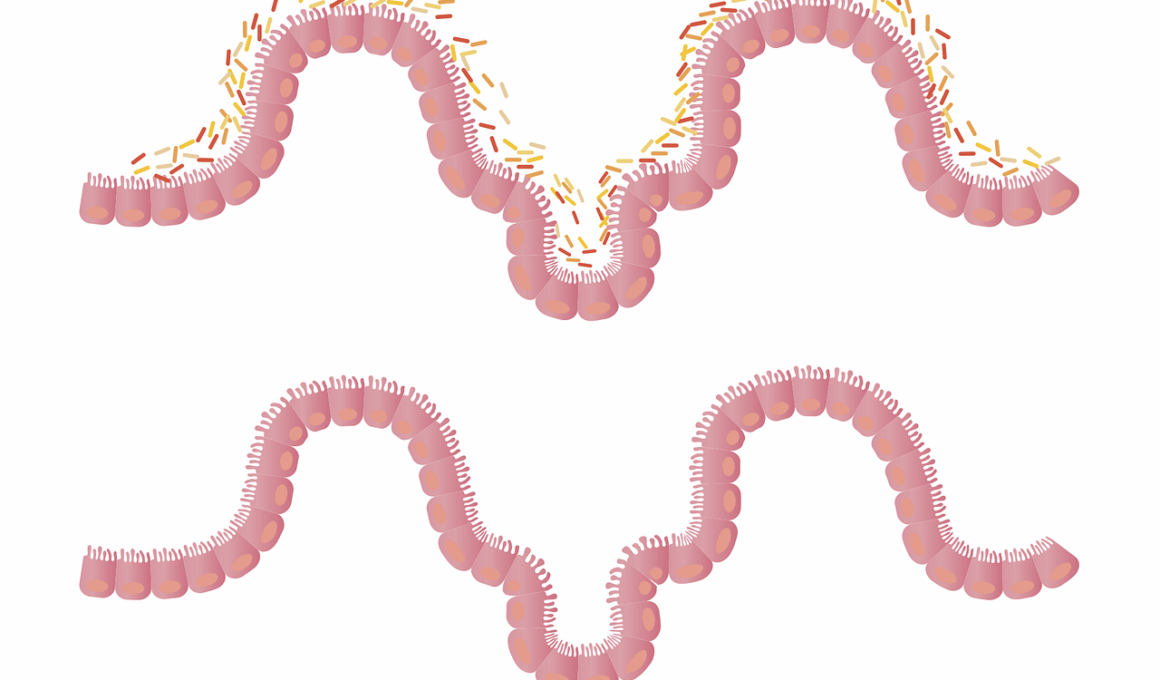
Antibiotics play a crucial role in treating various infections, however, they may also impact mental health through alterations in gut flora. The gut microbiome consists of trillions of microorganisms, and a healthy balance is essential for both physical and mental well-being. Antibiotics can disrupt this balance, leading to a condition known as dysbiosis. When dysbiosis occurs, the beneficial bacteria are diminished while harmful bacteria may flourish. This shift can result in various negative health outcomes. Research indicates a close connection between gut health and mental health, often referred to as the gut-brain axis. This axis emphasizes how gut microbes can influence brain activity, mood, and behavior. Disrupting gut flora with antibiotics may cause a cascade of mental health issues, including anxiety and depression. Recent studies have shown that individuals prone to mental health disorders may be particularly vulnerable to these changes. The consequences may be long-lasting, affecting mood regulation and stress response. Understanding the intricate relationship between antibiotics, gut flora, and mental health is essential for developing effective treatment plans and preventive strategies.
The gut-brain axis highlights the bidirectional communication between the gut and the brain. This communication is facilitated by various pathways, including neural, hormonal, and immune connections. The vagus nerve serves as a primary pathway in this communication, transmitting signals from the gut to the brain. When gut flora is imbalanced due to antibiotic use, signals transmitted along the vagus nerve may also be disrupted. Research shows that certain bacterial strains can produce neurotransmitters, such as serotonin and dopamine, which directly affect mood and cognition. A depletion of these beneficial bacteria due to antibiotics could lead to reduced serotonin levels, impacting overall mental health. Studies have shown that individuals taking antibiotics experience a higher risk of developing mood disorders. For instance, a significant correlation exists between antibiotic use and an increased incidence of anxiety and depression. Furthermore, the time and dosage of antibiotic treatment may influence the degree of these effects. While antibiotics are necessary for fighting infection, awareness of their potential impact on mental health is essential. Individuals should discuss these concerns with healthcare providers, weighing the benefits against potential mental health risks.
Long-term Effects of Antibiotics on Gut Flora
Repeated antibiotic use can lead to long-term alterations in gut flora composition, which may have persistent effects on mental health. Studies have shown that even after medical treatment concludes, imbalances in gut microbiota can remain for months or even years. These longstanding changes can perpetuate mood instability and anxiety levels. Prolonged dysbiosis can prevent a full recovery of gut health, leading to chronic gastrointestinal symptoms or disorders. It is essential to recognize a connection between chronic digestive issues and mental health problems. Research indicates that individuals with gastrointestinal disorders also tend to have a higher incidence of anxiety and depression. Moreover, young children and adolescents are particularly susceptible to the lasting effects of antibiotics on developing microbiomes. Early disruption can negatively impact their cognitive and emotional development, resulting in long-term mental health issues. Healthcare professionals must take these risks into account when prescribing antibiotics for children. Exploring alternative treatments or supportive therapies may be necessary to mitigate negative impacts. Further research is needed to establish definitive guidelines for antibiotic use and mental health considerations alongside gut health.
Restoring gut health post-antibiotic treatment is vital for supporting mental well-being. Probiotics and prebiotics have gained attention for their therapeutic potential in restoring a healthy gut microbiome. Probiotics are live beneficial bacteria that can help replenish lost gut flora, while prebiotics serve as food for these bacteria, promoting their growth. Studies have shown that the targeted use of specific probiotic strains can significantly improve gut health and mental health outcomes. Regular consumption of fermented foods, such as yogurt, kefir, and sauerkraut, can also be effective in promoting gut health. Additionally, dietary changes can help foster a healthy microbiome. Increasing fiber intake, particularly from fruits, vegetables, and whole grains, encourages the growth of beneficial bacteria. Reducing sugar and processed food consumption is equally important since these foods can promote harmful bacteria growth. Nutritional interventions combined with probiotics may amplify their efficacy. Mental health professionals should collaborate with dietitians to create comprehensive treatment plans that incorporate both psychological therapy and dietary strategies. The holistic approach emphasizes the interdependence of gut health and mental well-being.
The Role of Lifestyle Factors
Lifestyle factors also play a crucial role in maintaining gut health and, consequently, mental health. Regular physical activity can influence gut microbiota composition positively, enhancing diversity among bacterial species. Aerobic exercises, in particular, have been linked to beneficial changes in the gut flora. Stress management strategies are equally vital, as chronic stress can further exacerbate gut dysbiosis. Engaging in mindfulness practices can help reduce stress levels. Improved emotional regulation contributes to a healthy gut microbiome and better overall wellness. Sleep quality is another essential aspect to consider; inadequate sleep can adversely affect gut health, leading to a negative impact on mental health. Consuming a balanced diet rich in nutrients will bolster gut health while supporting physical and mental wellness. Moreover, avoiding smoking and limiting alcohol consumption has shown positive effects on gut health. Understanding the interplay between lifestyle choices, gut microbiome health, and mental health can lead to effective preventative strategies. Awareness of these connections empowers individuals to make informed decisions to improve their mental wellness and overall health outcomes.
The emerging research surrounding the gut-brain axis presents new avenues for mental health treatment. Integrative approaches that encompass both gut and mental health are becoming increasingly essential. Medical professionals may consider monitoring gut health in patients presenting with mental health disorders. Knowledge of a patient’s gut health could provide critical insights into their mental health history. Customizing treatment options that include dietary interventions alongside conventional therapy could enhance overall effectiveness. Novel therapies targeting the gut microbiome, such as fecal microbiota transplantation, are gaining interest as potential solutions. These innovative approaches aim to restore balance to the gut and improve mental health outcomes significantly. Continued research on the gut-brain connection is imperative for providing deeper insights into these phenomena. Understanding how antibiotic use can disrupt this connection is pivotal in formulating more effective treatments. Clinicians need to stay updated on this evolving field, developing strategies that promote gut health while effectively addressing mental health concerns. This multi-faceted perspective offers hope for better mental health management through improved understanding and care for gut health.
Conclusion and Future Perspectives
The link between antibiotics, gut health, and mental health cannot be ignored. Increased knowledge regarding this relationship is vital in managing both physical and psychological health effectively. As research evolves, clinicians will be better equipped to understand the implications of antibiotics on gut flora and mental wellness. Combining traditional medical therapies with supportive nutritional and lifestyle interventions offers significant promise. A greater focus on preventive strategies is warranted, particularly for populations at risk of experiencing mental health issues due to antibiotic treatment. Emphasizing an integrative approach can empower individuals to take charge of their health. Improvements in mental health management hinge on recognizing the complexities in our health systems, particularly the interactions of the gut. Education about mindful consumption of antibiotics, coupled with an understanding of the roles of gut flora, can lead to better health outcomes. As we confront future health challenges, a holistic view that incorporates both gut and mental health perspectives will be essential. It’s time to foster greater collaboration within the healthcare community to address the multifaceted nature of these connections.
In summary, a nuanced understanding of the relationship between antibiotics, gut health, and mental health is crucial in modern healthcare. By recognizing the profound impact that the gut microbiome has on mental well-being, strategies can be developed to mitigate risks associated with antibiotic use. Future research will undoubtedly uncover further connections and inform guidelines to improve treatment approaches, thereby ensuring the dual focus on physical and mental health. The path to well-being encompasses a holistic perspective, acknowledging the interdependence of all bodily systems. It’s imperative to prioritize gut health to support mental health, especially in vulnerable populations. Adopting lifestyle changes and integrative therapies offers significant benefits and fosters better health outcomes. Increasing awareness and education on these matters will empower individuals in their health journeys. Ultimately, understanding that our physical and psychological states are intricately linked enables us to approach health in a compassionate and informed manner. It’s a journey that requires collaboration, dedication, and a commitment to better health choices for ourselves and future generations. Embracing this approach could pave the way for more effective mental health solutions.