Inflammation, Gut Health, and Their Role in Obesity
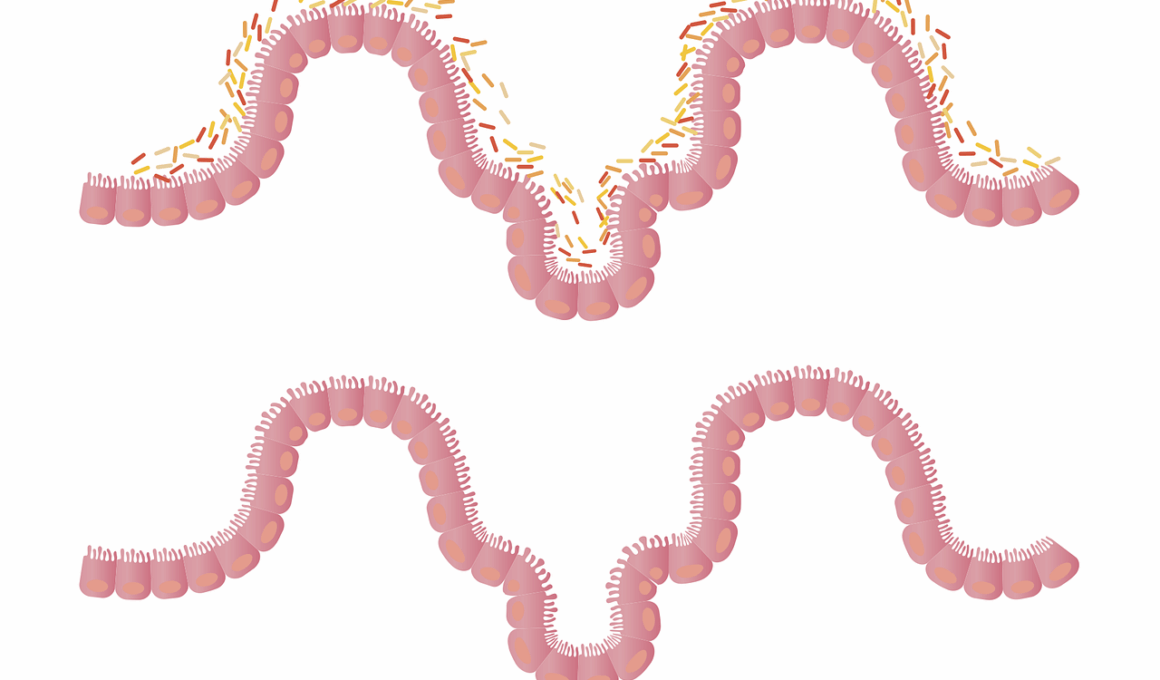
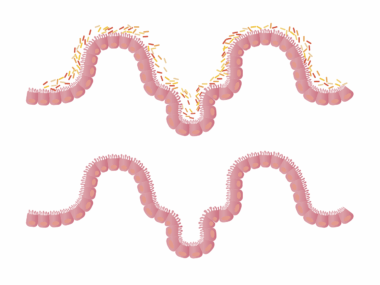
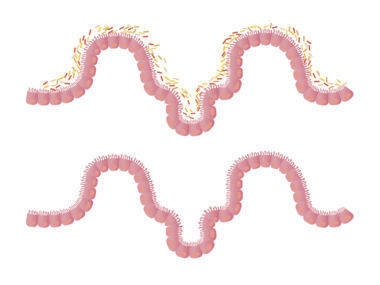
Understanding the complex relationship between inflammation, gut health, and obesity is crucial. Recent studies indicate that inflammation plays a pivotal role in the onset of obesity and associated metabolic disorders. Chronic low-grade inflammation is often linked with obesity, characterized by the overproduction of pro-inflammatory cytokines. One significant aspect is the gut microbiome, a vibrant ecosystem of microorganisms crucial for maintaining gut health. An imbalance in this microbiome can lead to increased intestinal permeability, often referred to as “leaky gut.” This condition allows toxins and undigested food particles to enter the bloodstream, triggering an inflammatory response. Thus, the state of the gut microbiome directly impacts systemic inflammation levels. Maintaining a healthy and diverse gut microbiome can help mitigate excessive inflammation and its consequences on weight management. Scientists suggest dietary choices significantly influence this microbiome, highlighting the necessity of incorporating fiber-rich foods, fermented products, and probiotics. This approach can enhance gut flora diversity, promote gut health, and help regulate body weight. Overall, understanding these connections highlights the need for lifestyle changes aimed at improving gut and immune health to manage obesity effectively.
Obesity and inflammation are deeply interconnected, affecting various bodily systems and processes. Adipose tissue produces inflammatory cytokines, which contribute to insulin resistance and metabolic syndrome. This creates a vicious cycle, as increasing inflammation leads to further weight gain. Individuals struggling with obesity often experience chronic inflammation, equipping them with a systemic disadvantage regarding metabolic health. One of the most effective interventions is to focus on the gut microbiota’s composition. Altering gut bacteria through diet can help reduce inflammation levels. Foods rich in omega-3 fatty acids, such as fish, and antioxidants found in fruits and vegetables can counteract inflammation. Furthermore, avoiding processed foods and excessive sugars contributes to a healthier microbiota. Exercise is another vital factor in managing inflammation alongside weight. Regular physical activity promotes beneficial gut bacteria diversity and reduces inflammatory markers in the body. Importantly, adequate sleep and stress management are necessary for maintaining low inflammation. Mental health impacts gut health significantly, establishing a connection through the gut-brain axis. Strategies combining dietary adjustments, exercise, and mental well-being can thus impact obesity by lowering inflammation and nurturing healthier gut flora.
The Gut-Brain Axis and Its Impact on Obesity
The gut-brain axis illustrates the intricate communication network between the gut and the brain, influencing eating behavior and metabolism. This connection is essential in understanding the role of gut health in obesity. The vagus nerve, which connects the brain to the gastrointestinal tract, plays a crucial role in transmitting signals that impact appetite and digestion. Hormones released during digestion, such as ghrelin and leptin, communicate energy status to the brain. Imbalances in these hormones are often seen in individuals with obesity. Moreover, gut microbiota can influence these hormonal responses, leading to increased hunger or reduced satiety. Consequently, a disrupted microbiome can result in overeating and weight gain. Research also indicates how stress affects this axis, potentially promoting unhealthy eating habits and influencing weight. When stressed, individuals may gravitate towards calorie-dense comfort foods, exacerbating weight issues. Psychological factors also contribute to gut health, as anxiety and depression can alter gut microbiota. Addressing the gut-brain axis through mindful eating, stress management, and nutritional therapies can significantly improve gut health and weight management outcomes.
Dietary choices profoundly influence gut health and obesity treatment. Consuming diverse and nutrient-rich foods enhances microbial diversity in the gut, promoting health. Probiotics, found in fermented foods like yogurt and sauerkraut, introduce beneficial bacteria to the gut, combating dysbiosis and inflammation. Prebiotics, sources of dietary fibers such as bananas and garlic, support beneficial bacteria by providing nourishment. A high-fiber diet fosters a flourishing microbiome, leading to improved gut health and metabolic balance. In contrast, Western diets, characterized by high sugar and fat content, harm gut microbiota diversity, often leading to inflammation and obesity. For successful weight management, incorporating whole grains, fruits, vegetables, nuts, and legumes is essential. These foods contribute to weight loss by promoting satiety and a healthy digestive system. Reducing processed food intake is equally crucial; these often contain additives that may disrupt gut health. A diet focused on whole, unprocessed foods not only supports healthy weight but also cultivates a favorable gut environment. Overall, optimal dietary strategies play a significant role in enhancing gut health and, consequently, in effectively managing obesity.
Factors Influencing Gut Health and Obesity
Several factors contribute to the deterioration of gut health, subsequently impacting obesity. Lifestyle variables such as diet, exercise, stress levels, and sleep patterns significantly influence gut microbiota composition. Unhealthy dietary habits, including excessive sugar and fat consumption, lead to an imbalanced gut flora, promoting obesity and metabolic disorders. Furthermore, lack of physical activity exacerbates gut health issues, as regular exercise fosters a diverse microbiome. Stress is another critical factor; heightened stress levels can affect digestion and gut function. Chronic stress can alter gut bacteria, leading to inflammation and weight gain. Sleep deprivation also plays a role; studies show insufficient sleep is linked to obesity through hormonal disruptions affecting appetite regulation. Medications, particularly antibiotics, can also adversely affect gut microbial diversity, leading to potential health complications. Individuals must be aware of these factors to adopt lifestyle changes that improve gut health. By addressing each aspect—from dietary choices to physical activity and mental health—people can reduce inflammation and manage their weight more effectively. Thus, understanding the multifactorial nature of gut health is crucial for obesity prevention and management.
One promising area of research involves the potential of certain foods and nutrients to support gut health in the context of obesity. Polyphenols, abundant in fruits, vegetables, teas, and spices, have shown anti-inflammatory properties. These compounds may enhance gut flora diversity and promote beneficial bacteria growth, leading to improved overall gut health. Foods rich in polyphenols include berries, green tea, and dark chocolate. Omega-3 fatty acids, primarily found in fish and flaxseeds, also play a crucial role in reducing inflammation. Integrating these foods into a balanced diet can have significant benefits. Additionally, research into the role of certain fibers, particularly resistant starch, highlights their potential to improve gut health. Resistant starch can be found in foods like cooked and cooled potatoes or legumes and is known to provide nourishment for beneficial bacteria. This increased fermentation in the gut can lead to an enhanced immune response and lower inflammation. Furthermore, maintaining adequate hydration is essential as it supports digestion and gut lining integrity. By emphasizing the incorporation of these nutritionally beneficial foods, individuals can enhance their gut health, reduce inflammation, and support effective weight management strategies.
Conclusion: The Path Forward for Gut Health and Weight Management
Given the complex interplay of inflammation, gut health, and obesity, a targeted approach can yield immense benefits. Recognizing that managing gut health is essential for tackling obesity is crucial. Implementing a multifaceted strategy, including dietary modifications, exercise, stress reduction, and proper sleep, can lead to improved gut microbiome diversity and reduced inflammation. It is essential for individuals to develop a sustained commitment to these lifestyle changes for optimal results. Incorporating a diverse range of foods, especially those high in prebiotics and probiotics, can make significant strides toward achieving better gut health. Staying informed about the latest research is vital as the fields of nutrition and microbiome studies evolve rapidly. An open-minded approach towards trials of various diets can reveal what works best for individual circumstances. Collaboration between healthcare professionals, nutritionists, and patients will foster holistic approaches and create sustainable weight management strategies. Through education and proactive lifestyle choices, individuals can effectively combat obesity and improve overall gut health. In this manner, significant strides toward health and well-being can be achieved for many.
Future Research Directions
The relationship between inflammation, gut health, and obesity is an area ripe for continued research. Future studies should focus on identifying specific gut microbes that play pivotal roles in inflammatory responses and weight management. Exploring dietary patterns allowing for more personalized nutrition could enhance interventions. Additionally, more extensive clinical trials evaluating the efficacy of specific probiotics for weight loss and inflammation management may yield valuable insights. Understanding how genetic predispositions interact with gut microbiota and diet will significantly enhance comprehension of obesity mechanisms. Investigating the gut-brain axis further could also unveil new treatment pathways, especially for those refusing conventional approaches. Effectively addressing gut health-related issues could open doors to novel therapeutic strategies in obesity treatment. Another viable aspect for research may include the impacts of environmental factors, such as pollution and urbanization, on gut health. As external elements affect microbiota composition, understanding these interactions could lead to innovative and holistic approaches in tackling obesity at a community level. Emphasizing gut health in public health policies may result in more comprehensive obesity management strategies. Comprehensive research can guide public health recommendations that support gut health.