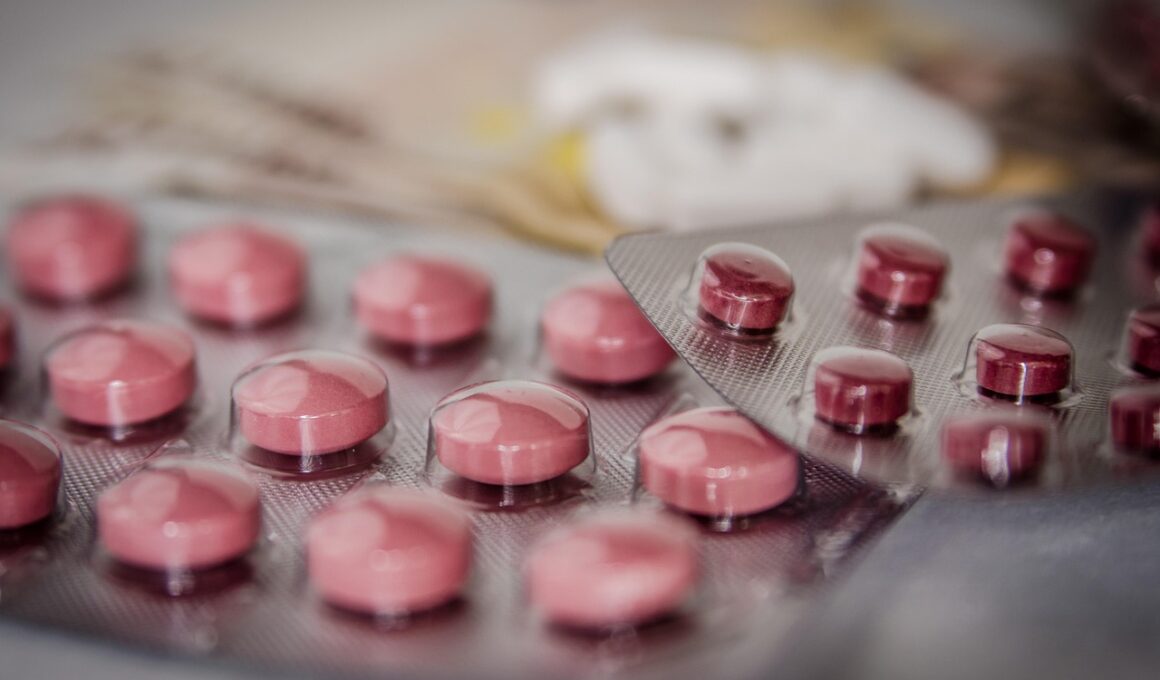
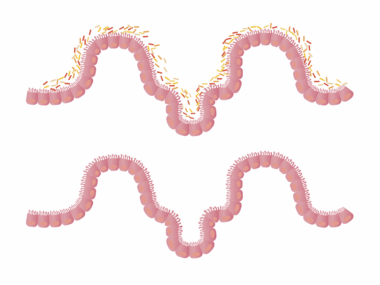
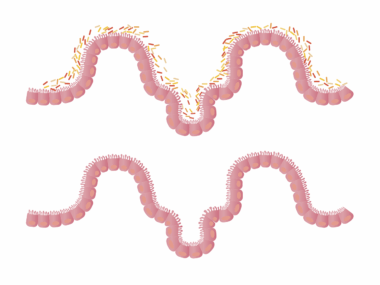
The Influence of Medications on Gut Microbiota
Medications can significantly affect the composition and function of gut microbiota, which plays a vital role in overall health. Antibiotics are among the most notorious for causing drastic changes, potentially leading to dysbiosis. Dysbiosis refers to an imbalance of microorganisms, which may result in gastrointestinal issues, obesity, and even autoimmune diseases. Other medications, such as proton pump inhibitors (PPIs), can also alter gut microbiome diversity. Studies have shown that PPIs not only change microbial composition but can also lead to an increased risk of infections. Moreover, corticosteroids, frequently prescribed for inflammation, can have similar impacts by altering the gut flora. Those taking these medications should remain vigilant about gut health. The implications of altered microbiota can be far-reaching, affecting digestion, absorption of nutrients, and immunity. Maintaining a balanced gut microbiome is essential, and this balance can be disrupted easily by certain drugs. The gut serves as a crucial link between the external environment and the immune system, so understanding medication impacts is necessary for better healthcare approaches. Further research is critical to establish guidelines for protecting gut health during medication usage.
In addition to antibiotics and PPIs, many chronic conditions lead to medication regimens that impact gut microbiota. Commonly prescribed medications like metformin, used in managing type 2 diabetes, have been shown to influence the gut microbiome positively. Research indicates that metformin’s mode of action may involve the modulation of gut bacteria, promoting beneficial strains. However, it is essential to examine the long-term effects of such medications on microbial communities. Other medications such as insulin therapy or statins may also influence microbial balance in the gastrointestinal tract. Observational studies have raised questions about the connection between statin use and certain microbiome profiles, suggesting that further investigations could yield significant insights. Medication-induced changes in gut microbiota can lead to alterations in drug metabolism and efficacy. This phenomenon highlights the importance of personalized medicine, where healthcare providers consider individual microbiome composition when prescribing medications. Understanding this link can optimize therapeutic outcomes. Future research is needed to uncover the intricate relationship between various medications and the gut microbiome. Improvements in microbiome health could potentially mitigate adverse effects associated with medications, positively influencing patient care further down the line.
Medications and the Immune System
A healthy gut microbiome not only aids digestion but also plays a critical role in modulating the immune response. Medications affecting gut microbiota can therefore have downstream impacts on immune function. Altered gut flora can lead to immune dysregulation, which may manifest as increased susceptibility to infections or autoimmune diseases. For example, the long-term use of antibiotics can diminish gut biodiversity, potentially leading to a compromised immune response. Research has demonstrated that a diverse microbiome is essential for proper immune development and function. Certain strains of bacteria present in the gut are known to enhance immune responses and help regulate inflammation. Conversely, medications that harm beneficial gut bacteria can impair these protective mechanisms and increase the risk of autoimmune disorders. It has been shown that the gut microbiome communicates with the immune system through various pathways, influencing how the body reacts to pathogens. Consequently, a careful assessment of the implications of medications on gut microbiota is essential for maintaining a balanced immune response. Future research is vital, focusing on restoring gut health when medications disrupt this equilibrium, thus promoting better health outcomes overall.
In the context of immune support, probiotics are emerging as a complementary approach to medications affecting the gut microbiome. Probiotics consist of live microorganisms that confer health benefits when consumed in adequate amounts. Numerous studies have demonstrated that probiotics can mitigate the adverse effects of antibiotic therapy, such as diarrhea and dysbiosis. Some strains of probiotics have shown potential in enhancing immune responses, promoting anti-inflammatory effects, and restoring microbial balance post-antibiotic treatment. Integrating probiotics into treatment regimens may aid in maintaining gut health even when medications disrupt microbial populations. However, it is essential to select the right probiotic strains, as not all provide the same benefits. Healthcare professionals must consider individualized approaches tailored to specific medications and health conditions. Additionally, dietary interventions can also play a crucial role in supporting gut microbiome health during medication use. Consuming a diet rich in fiber, prebiotics, and fermented foods can provide necessary substrates for beneficial bacteria. This synergistic approach emphasizes the importance of a comprehensive view of health that incorporates dietary choices alongside pharmacological interventions. Ongoing research will help clarify these complex interactions and guide future health strategies.
Long-Term Implications of Medication Use
Evaluating the long-term implications of medication use on gut microbiota is becoming increasingly important. Chronic medication use, especially during critical development periods like childhood or old age, can lead to significant and lasting changes in gut composition. Long-term effects sometimes manifest over years or even decades, leading to chronic gut conditions or systemic diseases. For instance, studies link prolonged PPI use with gut infections and alterations in microbiome diversity, suggesting that long-term reliance on such medications could be detrimental. Moreover, understanding these long-term implications will help clinicians make informed choices regarding patient treatments. Acquiring knowledge about the cumulative effects of medication on both gut microbiota and immune responses also presents opportunities for new therapies. Personalized medicine continues to gain traction, allowing tailored treatments that minimize adverse health risks associated with medication-induced dysbiosis. These considerations necessitate interdisciplinary collaboration between healthcare providers, researchers, and nutritionists to develop holistic care strategies. By understanding how medications interact with gut health, we can foster improved therapeutic outcomes for patients and enhance their overall well-being in the long run.
Furthermore, raising public awareness about the implications of medications on gut microbiota is crucial for promoting proactive health management. Patients should be informed about potential side effects and encouraged to communicate openly with healthcare providers about their medication regimens. By educating individuals about the importance of gut health and its relationship to overall well-being, we create opportunities for better health outcomes. Open discussions can pave the way for integrating lifestyle modifications alongside pharmacological treatments. Patients can be advised on lifestyle factors, including nutrition, exercise, and stress management, to support gut health. Increased awareness can also promote the use of probiotics as adjunct therapies, further benefiting the gut microbiome. Healthcare systems should prioritize educating both patients and professionals on this subject, fostering an environment that values gut health as part of comprehensive care. Ultimately, empowering patients with knowledge can encourage proactive health decisions that lead to better management of existing conditions and improved quality of life. Community initiatives that advocate for healthy gut microbiomes contribute to building a healthier society as a whole. The interplay between medication and gut health deserves attention and a commitment to further research and awareness.
Future Directions in Research
Moving forward, research on the interactions between medications and the gut microbiota must explore diverse areas for holistic understanding. Future studies should aim to clarify how various drug classes impact microbial communities and the potential for recovery after cessation. Also, analyzing how genetic variations in individuals influence responses to medications and their microbiome can enable personalized treatment strategies. Investigating the gut-brain axis is another emerging research frontier. Understanding the connection between gut microbiota, medications, and psychological health can yield novel insights into treating mental health disorders. The utilization of cutting-edge technologies such as metagenomics and machine learning can facilitate large-scale studies that track microbiome changes over time across diverse populations. Furthermore, clinical trials that investigate the combination of medications and probiotics could provide valuable data on optimizing treatments tailored to individual microbiome profiles. Finally, regulatory policies need to adapt, emphasizing the importance of microbiome health in drug development. Establishing guidelines that prioritize assessing gut impacts during drug testing will ensure safer therapeutic options. By addressing these research avenues, we can foster health-enhancing practices that improve patient outcomes and promote wellness.
In conclusion, the influence of medications on gut microbiota and immune system interactions is a complex and vital area of study. Acknowledging how medications like antibiotics, PPIs, and other common prescriptions impact gut health unveils the need for a multifaceted approach to healthcare. As we advance our understanding of these interactions, integrating probiotics and dietary changes into medication regimens may enhance therapeutic outcomes. Furthermore, empowering patients through education about their health plays an essential role. Long-term implications of medication use on gut microbiota must be examined closely to guide clinicians in making informed decisions about treatment options. Future research focusing on personalized medicine can offer tailored approaches that prioritize the gut microbiome’s integrity while considering individual variances in medication efficacy. As we highlight the importance of gut microbiota in overall health, we create a foundation for improved healthcare practices worldwide. Researchers, healthcare providers, and patients must work collaboratively to prioritize gut microbiome health. By emphasizing this connection, we can work towards developing targeted strategies that enhance well-being while minimizing complications arising from medication use and preserving gut health.