Does Sugar Cause Gut Inflammation? Evidence and Insights
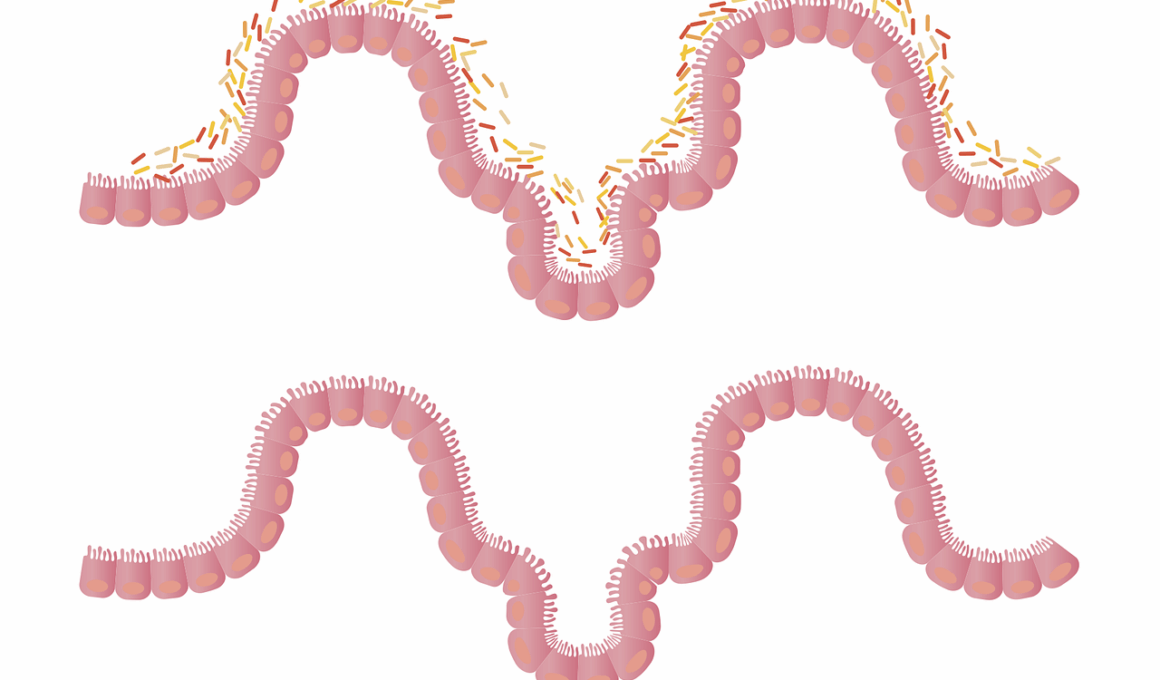
The relationship between sugar intake and gut inflammation has garnered significant interest in nutritional science. Recent studies suggest that high sugar consumption may alter gut microbiota, potentially leading to inflammation. The gut microbiome, comprising trillions of microorganisms, plays a crucial role in human health. It helps in digestion, nutrient absorption, and immune function. When we consume excessive sugars, particularly fructose and sucrose, harmful bacteria may proliferate, disrupting the balance of beneficial microbes. This imbalance can lead to an increased intestinal permeability, commonly referred to as ‘leaky gut’. Furthermore, sugar can promote the growth of inflammatory bacterial strains, exacerbating chronic inflammation in the gut. Chronic inflammation is linked to various digestive disorders, including irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD). Thus, there is a compelling argument that reducing sugar intake could be beneficial for gut health and may alleviate inflammatory responses. Awareness of sugar’s impact is essential not only for gut health but also for overall well-being. Future research is crucial to fully understand the dynamic interplay between sugar consumption, gut microbiota, and inflammation.
The Mechanism Behind Sugar-Induced Inflammation
Understanding the mechanism behind sugar-induced inflammation is critical in understanding its effects on gut health. When sugar enters the digestive system, it undergoes fermentation, leading to the production of certain metabolites. These metabolites can stimulate the immune system. An overactive immune response can, in turn, lead to chronic inflammation. The presence of high fructose corn syrup and refined sugars in many processed foods can be particularly harmful as they increase inflammation more than natural sugars found in fruits. Inflammatory cytokines released during sugar metabolism can further alter gut microbiota composition, encouraging pathogenic strains to flourish. One notable effect is the increased production of reactive oxygen species (ROS), which can damage gut cells and worsen inflammation. Importantly, evidence indicates that higher sugar diets are associated with increased risks of conditions such as metabolic syndrome and type 2 diabetes. Research supports that by reducing processed sugars, individuals may promote a healthier gut environment. Therefore, it is essential to consider dietary choices and their long-term effects on inflammation and gut health.
Moreover, the consumption of high sugar foods and beverages can lead to dysbiosis, which is an imbalance in the gut microbiome. This imbalance has been implicated in not only digestive disorders but also various systemic diseases. For instance, when beneficial bacteria are diminished, harmful bacteria can dominate, releasing toxins that further provoke an inflammatory response. Findings from studies indicate that the reduction of sugars can help restore balance in gut microbiota, leading to a healthier gut. Probiotics and prebiotics often complement a reduced-sugar diet by fostering the growth of positive gut bacteria. Additionally, individuals experiencing symptoms related to gut inflammation, such as bloating or fatigue, might find relief by being mindful of their sugar intake. Alongside cutting back on sugary foods, including more fiber-rich foods can support gut health and improve the microbiome’s resilience. Therefore, understanding these dynamics allows for more informed choices concerning diet and gut health management.
Evidence Supporting Sugar Reduction for Gut Health
There is accumulating evidence supporting the notion that reducing sugar can have positive effects on gut health. Several studies have examined the gut microbiome’s response to sugar reduction. For instance, one study highlighted that participants who reduced their sugar intake noted significant improvements in markers of inflammation and gut balance. Reports revealed an increase in beneficial gut species such as Bifidobacteria and Lactobacilli following sugar reduction interventions. These species are crucial for digestion and maintaining a robust immune system. Furthermore, other studies demonstrated that individuals with lower sugar diets showed fewer symptoms of gastrointestinal discomfort. This alignment reflects how dietary changes directly influence gut health outcomes. Additionally, researchers have pointed out that avoiding processed sugars decreases the risk of metabolic conditions linked to inflammation. The long-term benefits of a low-sugar diet can enhance overall health and well-being. Consequently, conducting more research into interventions promoting sugar reduction can further underscore the importance of diet on gut health and systemic inflammation.
Incorporating more whole foods and reducing sugar intake can lead to better body functioning and gut health. Whole foods, including fruits, vegetables, whole grains, and lean proteins, provide essential nutrients that support gut health without contributing to inflammation. These foods help nourish beneficial bacteria while avoiding added sugars that promote dysbiosis. Strategies such as mindful eating and meal prepping can aid individuals in making healthier food choices. It’s essential to read food labels, paying close attention to hidden sugars in products often perceived as healthy, such as yogurt or granola bars. Understanding added versus natural sugars can empower consumers, allowing them to prioritize their health and wellness effectively. Strategies may include gradually decreasing sugar intake to avoid overwhelming changes. Combining substitutions, such as using cinnamon for sweetness, can cut down sugar without sacrificing flavor. Beyond personal health, communities can benefit from awareness around sugar reduction. Access to education and resources will empower individuals to make informed dietary choices that may prevent gut inflammation and support overall health.
Conclusion on Sugar and Gut Inflammation
In conclusion, the evidence suggests that excessive sugar consumption is linked to gut inflammation and dysregulation of gut microbiota. This link reiterates the significance of considering dietary choices to manage inflammation and promote gut health. Following a balanced diet low in processed sugars while incorporating whole foods can yield notable health benefits. Awareness begins with understanding the adverse effects of sugar on gut function. For individuals experiencing gut-related symptoms, reducing sugar intake may be an effective step toward relief. Moreover, the broader implications of sugar reduction for community health cannot be ignored. Efforts to educate and implement strategies encouraging reduced sugar consumption can foster healthier populations. The ongoing differences between refined and natural sugar must also be highlighted within public health conversations, ensuring consumers can make the best choices for their well-being. As research continues to evolve, exploring the intricate connections between sugar, gut health, and inflammation remains essential. In summary, making dietary adjustments can fortify gut health and overall wellness, fundamentally enhancing the quality of life.
Lastly, nutritional guidance and support should be accessible for those looking to embrace a sugar-reduced lifestyle. Professionals can help in creating manageable plans to transition to healthier habits sustainably. By emphasizing moderation rather than complete elimination, individuals are more likely to succeed long-term. Incorporating behavior modification strategies such as journaling dietary intake could also help in maintaining accountability. Complementing dietary changes with regular physical activity can further improve gut health by enhancing digestion and promoting balance in the microbiome. Encouragement to access community resources such as workshops or cooking classes is crucial for supporting dietary changes. Not only do shared experiences enhance motivation, but they also provide a platform for further education about the effects of nutrition on health. As society becomes increasingly aware of the detrimental effects of sugar, a collective movement towards healthier nutrient choices can create a lasting impact. Ultimately, prioritizing gut health through reduced sugar intake is a viable path toward improved chronic disease management and enhanced overall well-being.
As we aim for a deeper understanding of how sugar affects our health, it is pivotal to integrate this knowledge into everyday practices. Collaboration between health care providers, policy-makers, and communities can establish more effective health strategies. The promotion of low-sugar diets can become part of public health initiatives to tackle widespread metabolic issues linked to sugar. Enhancing the availability of whole foods and eliminating food deserts can significantly impact community health outcomes. The role of sugar in gut inflammation presents a critical need for continued research and public awareness campaigns. If efforts are made to encourage healthier dietary patterns, the potential to reduce healthcare costs associated with sugar-related diseases becomes a possibility. The future of gut health relies on individuals becoming informed advocates for their dietary choices. Recognizing the powerful connection between what we consume and how we feel empowers people to take control of their health journey. As the landscape of nutritional science evolves, examining the relationship between sugar and gut health can lead to transformative insights that benefit society in profound ways.