Understanding the Link Between Gut Health and Neurodegenerative Diseases
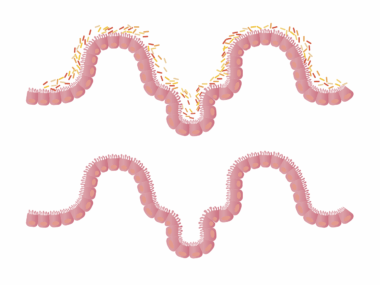
The gut microbiome, a complex community of trillions of microorganisms, plays a critical role in maintaining overall health. Recent studies have suggested a profound connection between gut health and neurodegenerative diseases, such as Alzheimer’s and Parkinson’s. The gut communicates with the brain through the gut-brain axis, influencing cognitive function and emotional well-being. Dysbiosis, or imbalance in gut bacteria, can lead to inflammation, which has been implicated in the progression of neurodegenerative disorders. Factors like diet, stress, and medication can disturb this balance. To promote a healthy gut microbiome, it’s essential to incorporate prebiotics and probiotics into your diet. Foods rich in fibers, such as fruits, vegetables, and whole grains, can serve as prebiotics, fueling beneficial bacteria. Probiotics, found in fermented foods, help replenish healthy gut flora. Moreover, regular physical activity and stress management techniques can also support gut health. Understanding the link between gut microbiome and mental health can offer new therapeutic avenues for managing neurodegenerative diseases. By prioritizing gut health, individuals may improve their cognitive resilience and overall quality of life.
Research has revealed the potential impact of the gut microbiome on neurodegenerative diseases, shedding light on the importance of gut health. For instance, individuals with Alzheimer’s disease often exhibit altered gut microbiota profiles compared to healthy controls. Some studies suggest that specific bacterial populations might influence neuroinflammation or amyloid plaque formation, both hallmarks of Alzheimer’s pathology. Additionally, other disorders like Multiple Sclerosis (MS) have been linked to gut dysbiosis, suggesting inflammation stemming from the gut can exacerbate neurological symptoms. Understanding these mechanisms brings hope for developing preventative strategies and therapies targeting gut health. Interestingly, the relationship between the gut and brain is bi-directional. Mood and mental health can be significantly affected by the composition of gut microbiota. Stress, anxiety, and depression can further disrupt gut health, which might create a vicious cycle. Furthermore, gut-derived metabolites produced by beneficial bacteria may exert neuroprotective effects, fostering cognitive function and mental wellness. Recent advancements in microbiome research open avenues for probiotics or dietary interventions as potential therapeutic options for neurodegenerative disorders. Exploring these possibilities may lead to more holistic and effective approaches to treatment.
Diet and Lifestyle Factors Affecting Gut Health
A well-balanced diet plays an indispensable role in maintaining a healthy gut microbiome. Consuming a diverse array of food promotes microbial diversity, which is crucial for optimal gut function. Diets rich in omega-3 fatty acids, antioxidants, and plant-based nutrients are particularly beneficial. These nutritional elements support not just gut health but overall wellness. Conversely, processed foods high in sugar and unhealthy fats can lead to dysbiosis, resulting in increased inflammation. Lifestyle choices, such as regular physical activity and sleep patterns, are also vital. Engaging in regular exercise can boost microbial diversity, enhancing gut-functioning. Furthermore, adequate sleep is essential for metabolic regulation and may support healthy gut microbiota composition. Managing stress is equally important; chronic stress can lead to changes in gut permeability, contributing to inflammatory processes. Meditation, yoga, and mindful breathing techniques can help manage stress levels effectively. Integrating these practices into daily routines may promote a healthier microbiome. An informed approach encompassing diet, exercise, and stress management establishes a robust foundation for a healthy gut, potentially mitigating the risk of neurodegenerative diseases.
Probiotics and prebiotics serve as key players in promoting a healthy gut microbiome, which can, in turn, influence neurological health. Probiotics, often referred to as “good bacteria,” can restore the balance of gut microbiota, while prebiotics provide nourishment for these beneficial organisms. Fermented foods like yogurt, kefir, sauerkraut, and kimchi are excellent sources of probiotics. Incorporating these foods into daily meals can help support gut health and improve overall well-being. In contrast, prebiotics found in garlic, onions, asparagus, and leeks serve as food for probiotics, enhancing their effectiveness. Recent evidence indicates that specific probiotics may hold promise for alleviating symptoms of anxiety and depression, which are commonly associated with neurodegenerative conditions. Furthermore, certain strains have demonstrated anti-inflammatory properties, which could be beneficial in mitigating neural inflammation pivotal in such diseases. Careful selection of probiotic and prebiotic sources is necessary to obtain desired health outcomes. Regular consumption of diverse, fiber-rich foods may support a thriving gut microbiome. These dietary choices create an environment conducive to improved brain health, contributing positively to the management of neurodegenerative diseases.
Future Directions in Research
As the understanding of the gut-brain connection expands, future research will likely focus on unraveling the complex interplay between gut microbiota and neurodegenerative diseases. Advances in microbiome sequencing technologies enable researchers to explore microbial communities more deeply. These insights may help identify specific bacterial strains that leverage protective effects against neurodegeneration. Clinical trials investigating the efficacy of targeted probiotics or dietary interventions could also yield valuable data, informing treatment guidelines for neurodegenerative conditions. Additionally, researchers will explore how environmental factors, lifestyle, and genetics influence microbial diversity and their relationship with neurological diseases. Innovative approaches, such as personalized nutrition based on an individual’s microbiome profile, may emerge as a significant focus. Personalized approaches will cater to each person’s unique microbial composition, ensuring optimal microbial health. Furthermore, studies on the mechanisms through which gut bacteria communicate with the nervous system will shed light on other potential intervention strategies. Understanding inflammatory pathways may also help identify biomarkers to predict neurodegenerative disease risk. As the research landscape evolves, these interdisciplinary efforts promise to pave the way for breakthroughs in managing gut health and its profound effects on neurological health.
Incorporating gut health into the discussion of mental health presents a paradigm shift in understanding neurodegenerative diseases. This approach highlights the intricate relations between physical health and mental wellness. Moreover, acknowledging emotional states’ effect on gut health serves as a reminder to maintain holistic health practices. Individuals experiencing anxiety and depression can benefit from considering their gut health as part of their overall treatment plan. Likewise, healthcare providers should be encouraged to adopt a more integrative approach, one that recognizes the importance of nutrition and lifestyle in mental health. Creating awareness will foster community support for preventive measures against neurodegeneration. Engaging in conversations within health communities is vital for sharing knowledge and experiences relating to gut health and its effect on brain function. Encouraging dietary education and the promotion of gut-friendly foods will empower individuals to make informed choices. Additionally, offering workshops or seminars focusing on gut health can enhance awareness surrounding these critical connections. Such initiatives can spark interest and encourage more individuals to take proactive measures. Ultimately, a collective effort toward understanding and prioritizing gut microbiome health can usher in significant advancements in mental health and neurodegenerative disease management.
Conclusion: Embracing a Holistic Approach
In conclusion, understanding the link between gut health and neurodegenerative diseases emphasizes the necessity of a holistic approach to wellness. Research continues revealing how dietary choices, lifestyle, and gut microbiota affect mental health. By actively promoting gut health through nutrition and lifestyle changes, individuals might mitigate the risks of neurodegenerative disorders. The interplay between the gut and brain offers promising avenues for future exploration. As we gain insights into specific bacteria that can influence brain health, the development of targeted therapies could transform treatment landscapes. Acknowledging the importance of mental health in conjunction with physical health is crucial for comprehensive care. This realization can drive further innovations in treatment modalities for neurodegenerative disorders. Creating a culture of awareness and proactive engagement is essential. Health professionals, patients, and communities must unite to prioritize gut microbiome health to foster better health outcomes and quality of life. By embracing holistic strategies that promote both gut and brain health, we can pave the way for a healthier future. Together, we can strive for improved cognitive function and reduced incidence of neurodegenerative diseases.
As the research unfolds, the potential for nutrition-led interventions targeting gut health progresses, offering hope for those affected by neurodegenerative diseases. Enhanced understanding of the gut-brain axis will warrant profound implications for therapeutic protocols in mental health care plans. Probiotic supplementation and an emphasis on prebiotic-rich diets may emerge as main components of comprehensive treatment regimens aimed at optimizing cognitive health. Health professionals should regularly evaluate gut health in individuals exhibiting early signs of neurodegeneration to better inform treatment. Potentially, early intervention through dietary modifications can yield significant benefits on cognitive decline progression. A community-based approach, focusing on public education surrounding gut health and its impact on mental well-being, will pave the way for proactive measures. Such initiatives can enhance overall mental health through encouraging better lifestyle choices. This could lead to increased awareness and engagement in maintaining a balanced gut microbiome. Continuous exploration in this field will ultimately contribute to establishing comprehensive guides for enhancing quality of life for individuals predisposed to neurodegenerative disorders. In summary, a unified approach prioritizing gut health is fundamental to enhancing brain health and well-being.