The Role of Personalized Nutrition in Managing Gut-Related Autoimmune Disorders
Gut-related autoimmune disorders affect millions, and personalized nutrition can play a crucial role in management. These disorders, such as Crohn’s disease or Hashimoto’s thyroiditis, arise when the immune system mistakenly attacks the body’s tissues, often leading to inflammation and other symptoms. Each individual may have a unique response to different foods, thus highlighting the need for customized dietary approaches. Personalized nutrition refers to tailoring dietary plans based on specific genetic, microbiome, and metabolic profiles of individuals. This method allows for a targeted approach, potentially decreasing inflammation and supporting gut health. Research indicates that specific dietary components can exacerbate or alleviate symptoms of autoimmune conditions. For example, gluten and dairy are often culprits for those with gluten sensitivity or lactose intolerance. By identifying these triggers through personalized testing and evaluation, individuals can significantly improve their quality of life. Eliminating or reducing inflammatory foods can lead to a decrease in symptoms, further supporting the body’s healing process. Collaboration with nutritionists and healthcare providers is essential in developing an effective personalized plan.
Understanding Gut Health and Autoimmunity
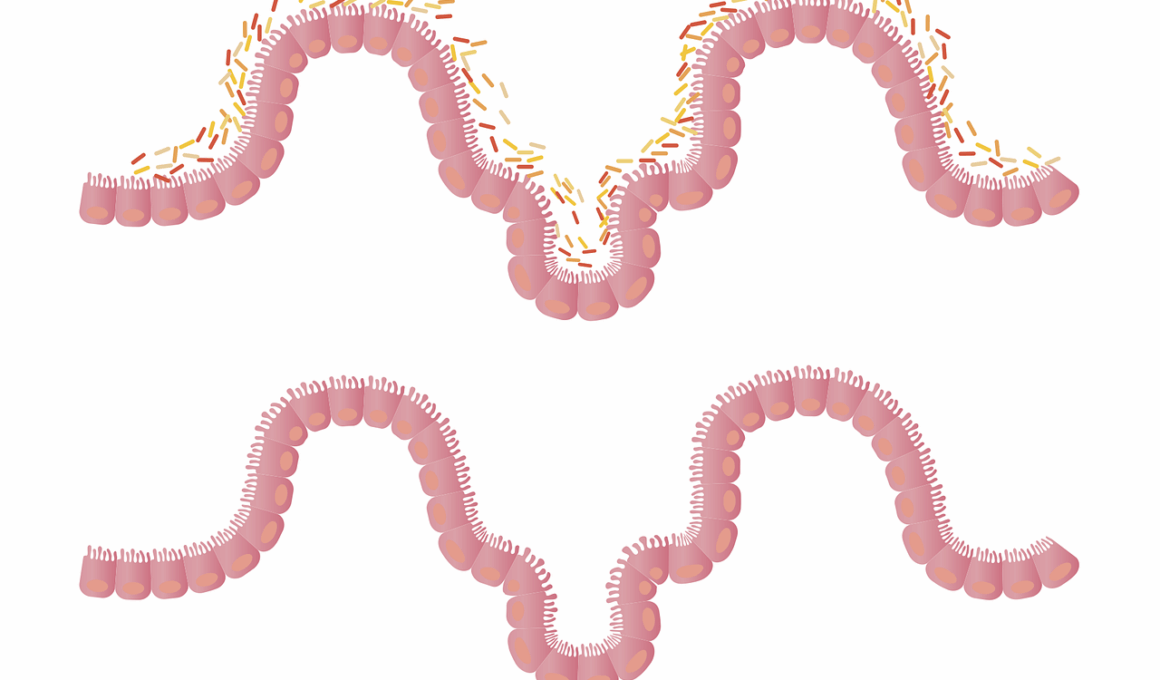
To understand the importance of personalized nutrition, it is vital to explore the connection between gut health and autoimmune disorders. The gut is home to trillions of bacteria, collectively known as the gut microbiome, which plays a significant role in overall health. A balanced microbiome aids digestion, supports immune function, and protects against pathogens. However, disruptions in this balance can trigger autoimmune diseases. Factors such as poor diet, stress, and environmental toxins can lead to dysbiosis, deteriorating gut health. This imbalance may increase intestinal permeability, often referred to as ‘leaky gut,’ allowing toxins to enter the bloodstream and triggering an immune response. Personalized nutrition strategies aim to restore gut health by addressing individual dietary needs. For instance, incorporating prebiotic and probiotic-rich foods can promote beneficial bacteria growth. Fermented foods like yogurt, sauerkraut, and kefir are excellent choices. Additionally, emphasizing anti-inflammatory foods such as fruits, vegetables, nuts, and fatty fish can further support gut healing. By prioritizing gut health, individuals with autoimmune disorders may experience reduced symptoms and enhanced overall well-being.
Incorporating personalized nutrition involves understanding one’s unique biochemical responses to food. For instance, certain individuals might have food intolerances or sensitivities that exacerbate gut inflammation. Comprehensive testing, including food sensitivity assessments and microbiome analysis, can provide valuable insights. Dietitians often recommend an elimination diet to identify food triggers, systematically removing and reintroducing items. This method helps personalize nutrition further to target inflammation proactively. Moreover, maintaining a food diary can assist in recognizing patterns related to gut health, helping individuals observe how different foods impact their symptoms. Besides identifying troublesome foods, some individuals may benefit from specific supplementation. Omega-3 fatty acids, for instance, are known for their anti-inflammatory properties and can be beneficial in managing symptoms. Nutritional strategies should not only be reactive but also preventative, helping to fortify the gut lining and immune system. Additionally, hydration plays a crucial role in digestion and nutrient absorption. Ensuring adequate water intake supports the movement of nutrients and aids in the elimination of toxins, further contributing to overall gut health and recovery from autoimmune conditions.
The Impact of Lifestyle on Gut Health
Beyond dietary choices, lifestyle factors significantly influence gut health and autoimmune disorders. Stress is known to affect gastrointestinal function adversely, leading to inflammation and gastrointestinal distress. Therefore, managing stress is essential through mindfulness practices, exercise, and relaxation techniques. Regular physical activity enhances gut motility and can foster a healthier microbiome. Yoga, walking, and other forms of moderate exercise have proven beneficial for reducing stress and improving gut function. Sleep is another critical aspect; insufficient sleep can disrupt gut health and exacerbate autoimmune symptoms. Aiming for 7-9 hours of quality sleep each night can support both physical and immune health. It is also crucial to limit exposure to substances that can harm gut health, including excessive alcohol and tobacco use. These substances can contribute to inflammation and negatively influence the microbiome. By adopting a holistic approach that prioritizes both nutrition and lifestyle, individuals may experience marked improvements in gut health. Personalizing this framework according to individual needs allows for better management of autoimmune disorders and contributes to a greater sense of well-being.
In conclusion, personalized nutrition offers a promising pathway for managing gut-related autoimmune disorders. With a tailored approach that considers an individual’s genetics, metabolism, and microbiome, dietary strategies can be optimized for healing. Recognizing the impact of specific foods can reduce inflammation and enhance overall gut health. Collaborating with healthcare professionals, including nutritionists or dietitians, ensures the development of a comprehensive plan addressing one’s unique needs. Additionally, lifestyle factors such as stress management, exercise, and proper sleep are crucial for maximizing gut health benefits. Understanding that gut health is interconnected with various bodily functions underscores the importance of a holistic outlook. The drive for personalized nutrition is not just about symptom alleviation; it is also about empowerment and advocacy for preventive health measures. Individuals with autoimmune disorders can take charge of their health by understanding their bodies better and making informed dietary choices. As research continues to evolve in the field of personalized nutrition, more evidence will support its effectiveness in managing complex autoimmune conditions. Embracing this innovative approach provides hope for improved health outcomes and enhanced quality of life.
Future Directions in Personalized Nutrition
The future of personalized nutrition lies in technological advancements and increased accessibility to nutritional genomics. Rapid developments in genetic testing allow individuals to understand their unique nutritional needs better. Additionally, mobile applications can assist people in tracking their diets, symptoms, and overall health. These technologies make it easier to manage personalized nutrition plans and provide guidance based on individual insights. Moreover, these approaches are likely to incorporate artificial intelligence for predictive analytics. AI can analyze comprehensive data sets, developing tailored nutrition plans based on past dietary habits and health outcomes. As awareness surrounding gut health and its connection to autoimmune disorders grows, more resources and funding will likely focus on research in this area. This could lead to new findings regarding specific dietary interventions, contributing further to understanding the gut-brain connection. Furthermore, community support and educational programs can empower individuals to make informed dietary choices, ultimately fostering a proactive approach to gut health. The integration of personalized nutrition with healthcare services can pave the way for innovative treatment options and approaches for managing autoimmune diseases.
The journey toward better gut health through personalized nutrition requires commitment and continuous learning. Individuals must stay informed about emerging research and adaptable nutrition strategies. Being engaged in one’s health journey through self-advocacy and education can make a world of difference. It is crucial for individuals to recognize that nutrition is not a one-size-fits-all approach. The integration of empirical research and individual experiences can provide a balanced view of effective dietary practices. Joining support groups or engaging in community workshops can enhance understanding and motivation. As individuals collaborate on exploring personalized nutrition, they can share insights and success stories. Ultimately, the path toward optimal gut health is not only about managing symptoms; it also involves fostering a deeper connection with one’s body and its needs. Continuing to refine and adapt dietary habits promotes resilience and empowers individuals to navigate the challenges posed by autoimmune disorders. A focus on personalized nutrition and holistic healing can lead to lasting positive changes in one’s overall health and lifestyle.