Tracking Gut Microbiome Changes After Bariatric Surgery in Diabetics
Bariatric surgery is an increasingly common intervention for obesity and type 2 diabetes management. Emerging studies indicate significant changes in gut microbiota after such procedures. The composition of gut microbiota can impact metabolic outcomes, with potential effects on insulin sensitivity. Tracking these microbiome changes may offer insights into the mechanisms underlying weight loss and diabetes remission. Following surgery, patients often experience shifts in their microbial diversity and abundance. Therefore, understanding these alterations can lead to targeted therapies. Research aims to define specific microbiome profiles associated with improved metabolic conditions. These profiles may help in predicting diabetes outcomes and postoperative success. Regular monitoring of gut health is essential for diabetic patients undergoing this surgery. Factors such as diet, lifestyle, and medication post-surgery play a crucial role in determining microbiome stability. Personalized nutritional plans may optimize gut health and enhance recovery. It is essential to consider that the relationship between the gut microbiome and diabetes is complex. Continuous research is needed to unveil mechanisms that contribute to metabolic changes in diabetic patients after bariatric procedures.
Understanding Gut Microbiome and Its Role in Diabetes
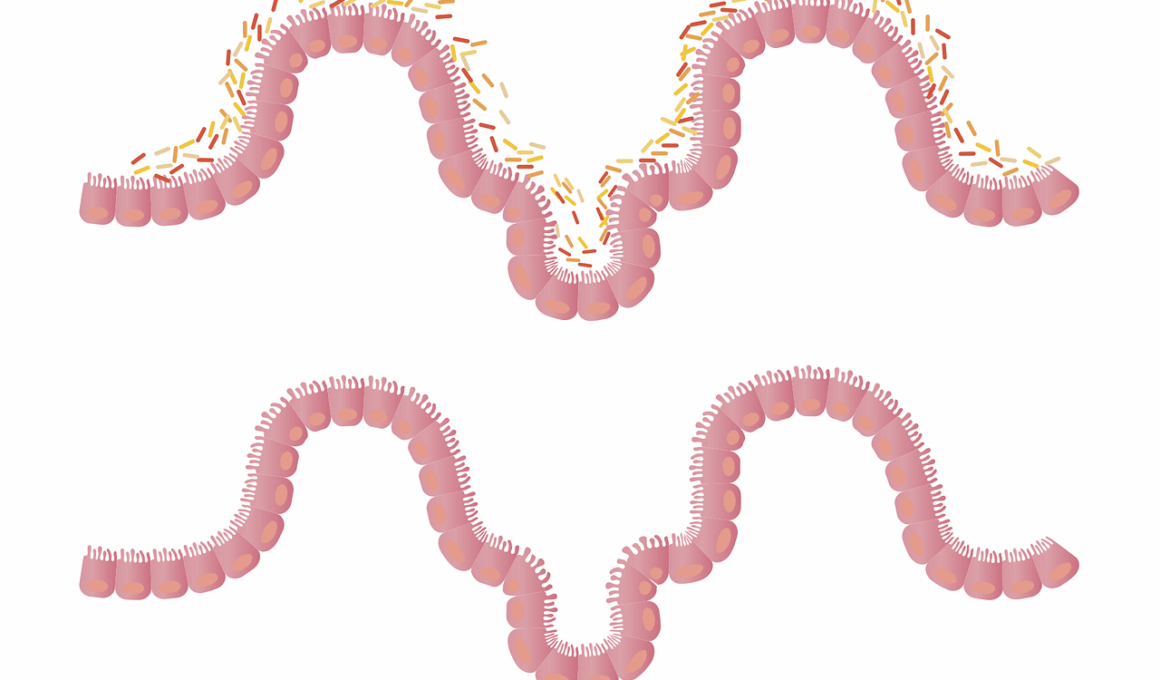
The gut microbiome refers to the vast array of microorganisms residing in the digestive tract. These microbes play a pivotal role in digestion, immune modulation, and metabolic regulation. Dysbiosis, or an imbalance in gut microbiota, is linked with various metabolic disorders, including obesity and type 2 diabetes. Emerging evidence suggests that gut health significantly influences glycemic control. Thus, understanding the gut microbiome’s role is vital for developing effective diabetes management strategies. Studies have shown that gut microbes can affect insulin sensitivity and inflammation processes. Certain beneficial bacteria may help regulate blood sugar levels by producing short-chain fatty acids. These substances improve gut health and have anti-inflammatory effects. Moreover, a diverse microbiome is generally associated with better metabolic health. Interventions such as diet modification and probiotics are being investigated for their potential to enhance microbiome diversity. It’s essential for diabetics to adopt a balanced diet rich in fiber and fermented foods to foster a healthy gut environment. Future research may reveal novel treatment avenues targeting gut microbiota to combat diabetes.
In recent years, bariatric surgery has gained attention as a viable treatment for obese individuals with type 2 diabetes. Surgical interventions such as gastric bypass alter the anatomy of the gastrointestinal tract, leading to significant weight loss and improved glycemic control. Patients often experience a dramatic reduction in insulin resistance following surgery. Observational studies report high rates of diabetes remission post-surgery. However, the impact of surgical techniques on gut microbiome composition is a focal area of research. Different types of bariatric surgeries may lead to distinct microbiota profiles, influencing postoperative outcomes. Researchers are exploring how these profiles correlate with improvements in metabolic health. Some studies have found that patients who undergo laparoscopic gastric bypass experience changes in gut flora leading to a higher diversity and abundance of beneficial bacteria. This microbial shift may enhance the body’s capacity to process nutrients efficiently. Furthermore, specific bacteria identified in the post-surgical microbiome might play crucial roles in weight loss and glucose metabolism. Continued research into personalized microbiome dynamics will aid in optimizing patient management for diabetic individuals undergoing surgery.
Long-term Implications of Gut Microbiome Changes
Monitoring changes in gut microbiome following bariatric surgery carries significant clinical importance. Understanding these changes helps predict long-term metabolic outcomes in diabetic patients. In some cases, microbiome alterations may stabilize over time or lead to dysbiosis, adversely affecting patient health. Regular follow-up and assessments of gut microbiota can identify patients at risk for metabolic complications. This knowledge empowers healthcare providers to implement timely interventions. Dietary modifications and supplementation with prebiotics or probiotics are potential strategies to enhance microbial diversity. Personalized approaches catered to individual microbiome profiles may optimize long-term weight management and glycemic control. This can improve quality of life and reduce the incidence of diabetes-related complications. Furthermore, the gut-brain axis’s involvement in metabolic regulation implicates gut health in broader health outcomes. Studies have shown that gut bacteria can communicate with the brain, influencing appetite and emotional well-being. Thus, ensuring a healthy microbiome may not only improve metabolic health but also mental health among diabetics. A holistic approach to patient care must consider these interactions for comprehensive management.
Research continues to delve into the relationship between gut microbiota and diabetes following bariatric surgery. One intriguing aspect is the influence of specific diets on gut bacteria composition. Low-carbohydrate or ketogenic diets, often adopted post-surgery, can fundamentally reshape the microbiome. These diet strategies emphasize reduced carbohydrate intake, potentially lowering blood sugar levels. As a result, diabetic patients may observe significant improvements in their glycemic control. Nutritional intake also plays an essential role in determining the success of microbiome modulation. Foods rich in probiotics, such as yogurt and fermented vegetables, can promote the growth of beneficial bacteria. Conversely, high sugar and processed foods may exacerbate dysbiosis, undermining surgical benefits. Another critical area of research focuses on the role of gut-derived metabolites in glucose metabolism. Short-chain fatty acids produced by gut fermentation may enhance insulin sensitivity and gut barrier functions. Hence, a thorough dietary strategy, focusing on gut health, helps support metabolic conditions in diabetics post-bariatric surgery. Ongoing investigations aim to solidify these relationships and establish dietary guidelines based on microbiome profiles.
Future Directions in Microbiome Research
The future of microbiome research holds great promise for diabetes management. Developing personalized medicine approaches may revolutionize treatment protocols for diabetics post-bariatric surgery. This involves tailoring dietary strategies based on individual microbiome profiles, optimizing patient-specific outcomes. Additionally, research is focusing on understanding the functional aspects of gut microbiota. Identifying key microbial species responsible for metabolic benefits may lead to innovative therapies. Moreover, advancements in microbiome analysis technology will enable us to gather more comprehensive data regarding gut health. This includes next-generation sequencing and metabolomics, leading to a better understanding of microbial functions in glucose metabolism. The implication is profound for formulating targeted probiotics or prebiotics that directly address dysbiosis in diabetic patients. Furthermore, integrating gut microbiome assessments into routine clinical practice may provide valuable insights into patient management. Clinicians can leverage this data to monitor microbiome health and intervene accordingly. In summary, the avenue of microbiome research is vast and uncharted, with potential benefits extending far beyond traditional diabetes management methods.
Ultimately, the interconnectedness between gut microbiota and diabetes highlights the necessity for multidisciplinary approaches. Gastroenterologists, endocrinologists, and nutritionists must collaborate to construct comprehensive care strategies. Monitoring gut health before and after bariatric surgery is essential for optimizing patient outcomes. Encouraging patients to engage actively in their health journey also enhances motivation and adherence to guidelines. As researchers unravel the complexities of the gut microbiome, a paradigm shift in diabetes management is on the horizon. Future interventions can become more personalized and targeted, improving effectiveness over generic approaches. Emphasizing lifestyle changes, including diet and exercise, alongside microbiome health plays a crucial role in achieving long-term success. With ongoing studies, more connections will likely be established between specific microbial functions and diabetes. The ultimate goal remains to transform the landscape of diabetes care and provide better quality of life for patients. As insights continue to be uncovered, the hope is for innovative solutions that address both microbiome health and metabolic conditions, ultimately leading to enhanced diabetic management.