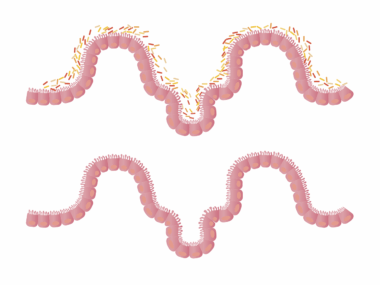
How Sugar Affects Chronic Digestive Conditions
Sugar plays a significant role in various chronic digestive disorders, affecting the gut in numerous ways. For individuals suffering from conditions such as irritable bowel syndrome (IBS) or inflammatory bowel disease (IBD), sugar can exacerbate symptoms, leading to increased bloating, gas, and discomfort. High sugar intake is linked to inflammation in the gut, which can worsen symptoms associated with digestive diseases. Many processed foods contain hidden sugars, making it essential for patients to read labels carefully. The types of sugars consumed can also make a difference. For example, fructose, found in many fruits and sweeteners, may not be tolerated by everyone and can induce digestive distress. Understanding the impact of sugar on gut health is crucial for managing symptoms. Moreover, it is vital to recognize that individual responses to sugar vary. Some people may tolerate modest amounts of sugar without issue, while others experience immediate negative effects. Identifying personal tolerance levels and adjusting dietary habits accordingly is essential for promoting gut health and overall well-being for those suffering from chronic digestive conditions.
The Link Between Sugar and Inflammation
Chronic inflammation within the gastrointestinal tract is a hallmark of many digestive disorders. Sugar can contribute significantly to inflammation through various pathways, inducing changes in gut microbiota and increasing the permeability of the intestinal lining. This can lead to what is known as “leaky gut syndrome,” where excessive sugar feeds pathogenic bacteria, leading to dysbiosis. As a result of this imbalance, the immune system may overreact, perpetuating inflammation. Furthermore, sugar triggers the release of pro-inflammatory cytokines, further complicating the body’s response to manage symptoms effectively. For those with chronic conditions like Crohn’s disease or ulcerative colitis, sugar can become a double-edged sword, providing temporary pleasure while ultimately harming gut health. Reducing sugar intake may help alleviate these inflammatory responses and support healing. Incorporating anti-inflammatory foods such as fatty fish, nuts, and leafy greens can also be beneficial. Regular monitoring of one’s diet to limit sugar intake can yield positive results in symptom management, with added benefits for overall digestive wellbeing. Changes do not have to happen overnight, but gradually cutting back on sugar can lead to significant health improvements in the long run.
Another important aspect to consider is the type of sugars consumed. Natural sugars, those found in whole fruits and some vegetables, are generally less harmful when compared to added sugars in processed foods. Nutritionally rich foods not only provide sugars but also essential vitamins and fiber, which can improve digestion. On the contrary, refined sugars found in candies, soft drinks, and baked goods lack nutritional value and can lead to further complications for those with digestive issues. Such sugars can ferment in the gut, causing discomfort, diarrhea, and other symptoms associated with IBS. The glycemic index is another factor to be wary of. Foods with high glycemic indexes can spike blood sugar levels rapidly, leading to various consequences for digestive health. Getting educated on the differences between types of sugars, and their potential impact on gut health, is vital for anyone managing chronic digestive conditions. Eliminating refined sugars while embracing alternatives can create a healthier path, not only reducing symptoms but also enhancing the body’s overall functioning. Consulting with a nutritionist can provide personalized guidance to tailor dietary choices accordingly.
Strategies for Reducing Sugar Intake
For patients struggling with chronic digestive disorders, effective strategies exist to cut back on sugar consumption. A great starting point is to identify all potential sources of sugar in the diet, including condiments, beverages, and packaged snacks. Reading food labels can unveil hidden sugars that sometimes escape notice. Once the sugar sources have been identified, substituting high-sugar foods with healthier alternatives becomes easier. For instance, swapping sugary cereals for oatmeal topped with fresh fruit can provide natural sweetness without the added sugar. Engaging in meal planning also helps manage sugar intake effectively, allowing for better control over what is consumed. Keeping healthy snacks on hand, such as nuts and yogurt, can prevent reaching for processed sugary snacks during cravings. Additionally, practicing mindfulness while eating can enhance awareness of food choices, helping to avoid impulsive decisions that lead to high sugar consumption. Reducing sugar doesn’t mean sacrificing taste; experimenting with spices like cinnamon or vanilla can add flavor without the calories. Remembering to stay hydrated is essential, as sometimes thirst is mistaken for hunger, leading to unnecessary snacking on sugar-laden foods.
Another major factor in managing sugar intake is understanding cravings. Recognizing when and why cravings occur can be beneficial in creating a tailored approach to resistance. For instance, many people find they crave sugar when they are bored, anxious, or tired. Finding healthier coping mechanisms, like exercise or meditation, can help manage those cravings more effectively. Keeping a food diary may also shed light on habits and patterns, allowing one to build strategies tailored to their needs. Seeking support from healthcare professionals specialized in nutrition can play a key role as well. They can provide personalized plans and support systems to effectively reduce sugar intake. Community support, whether through online forums or local support groups, can also help in maintaining motivation. Another method involves learning to enjoy naturally sweet flavors through fruits or sweet-tasting vegetables, creating a pleasurable experience in healthy eating. The focus should remain on balance, aiming for moderation rather than perfection. The journey of modifying dietary habits may take time but can lead to long-term health benefits for digestive function. Small, sustainable changes can create lasting impact on overall well-being.
Conclusion
Understanding how sugar impacts chronic digestive conditions is a crucial aspect of managing symptoms effectively. From inflammation to gut microbiota imbalance, sugar overwhelms the system, creating challenges for those coping with chronic illnesses. Recognizing the sources of sugar, differentiating between types, and reducing overall intake are essential first steps for reducing symptoms and promoting healing. Each individual’s experience is unique, thus requiring personalized strategies and approaches to successfully navigate dietary changes. Consulting healthcare professionals and engaging with supportive communities can empower individuals on their journey towards better gut health. The relationship between sugar and chronic digestive conditions is complex and must be approached mindfully. While sugar adds sweetness to life, its overconsumption can lead to significant health challenges. By prioritizing nutritious foods and adopting sustainable dietary strategies, it is possible to manage symptoms effectively. Ultimately, fostering a balanced relationship with food, including occasional indulgences, can ensure overall happiness while safeguarding digestive health. As awareness continues to increase regarding the negative effects of sugar, proactive measures must be taken to ensure a healthier future.
In conclusion, sugar significantly affects chronic digestive conditions, making it vital to approach consumption with caution. Individuals experiencing chronic digestive issues must strive for dietary changes that support gut health and reduce inflammation. This approach involves identifying and understanding patterns, sources, and types of sugars consumed daily. The impact of sugar on inflammatory responses in the gut should not be underestimated, as it influences long-term health outcomes. Patients are encouraged to consult with healthcare professionals to develop personalized strategies tailored to their specific needs. Alongside individual efforts, seeking community support can also enhance commitment. Regular monitoring and adjusting dietary habits can yield significant benefits for digestive health. The process may require patience and diligence, but an enhanced quality of life can emerge from reducing sugar intake. Embracing whole foods and focusing on nutrient-rich choices can reverse the adverse effects of sugar overconsumption. It is crucial to remember that managing chronic digestive conditions is an ongoing journey, and success comes from taking empowered, informed steps toward achieving optimal gut health.
Maximizing health begins with recognizing the influence of sugar on our bodies. This is especially true for individuals with chronic digestive issues, who must navigate their dietary choices mindfully. Together, small, repeatable changes can have significant impacts on overall health. Exploring various flavor profiles, accessing reliable information, and engaging with supportive communities can enhance individual experiences. Maintaining a balanced approach should remain the ultimate goal while ensuring that every decision recognizes the impact of our food choices. Fostering sustainable habits promises brighter days for those struggling with chronic digestive disorders. Taking initial steps might seem daunting, but positives await those committed to lasting changes in their diets. As families, friends, and communities unite to support dietary changes, awareness about the effects of sugar will continue to grow. A revitalized focus on nutrition can knit closer ties between individuals and their food, creating a more harmonious relationship. The future of gut health begins with us, and choosing healthful options will lay the foundation for happier lives.