The Connection Between Gut Dysbiosis and Insulin Resistance
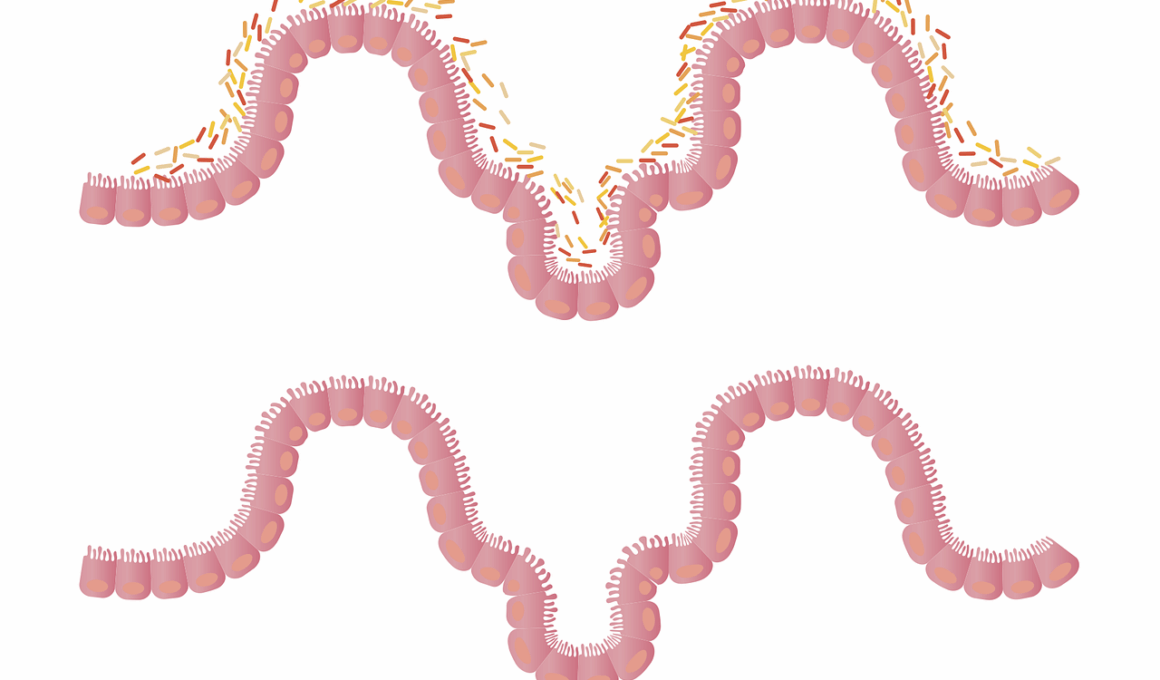
The human gut hosts trillions of microorganisms known as the gut microbiota, which play a pivotal role in overall health. Emerging studies indicate a significant link between gut dysbiosis, an imbalance in these microorganisms, and insulin resistance. Insulin resistance is a condition where the body’s cells become less responsive to insulin, leading to elevated blood glucose levels. This scenario poses a risk for developing type 2 diabetes, a major health crisis globally. Gut dysbiosis may influence insulin resistance through various mechanisms, including alterations in inflammatory pathways and metabolic processes. Inflammatory responses caused by harmful gut bacteria can release cytokines that interfere with insulin signaling pathways. Furthermore, an imbalance in the microbiota may disrupt short-chain fatty acid production, essential for metabolic health. Additionally, specific gut bacteria may influence the body’s metabolism of glucose and fats. Therefore, promoting gut health through diet and lifestyle changes is crucial. A diverse diet rich in fiber can help restore a healthy gut microbiome. Foods like fruits, vegetables, and whole grains can support beneficial bacteria, promoting metabolic health and reducing insulin resistance.
Impact of Diet on Gut Health
Diet plays an essential role in maintaining gut health and potentially preventing insulin resistance. Foods high in fiber, prebiotics, and probiotics contribute significantly to the diversity and abundance of beneficial gut bacteria. Consuming a diet filled with whole foods encourages a healthy microbiome that can efficiently regulate metabolic processes. On the other hand, diets high in processed sugars and fats can lead to gut dysbiosis, promoting undesirable bacteria and exacerbating insulin resistance. Research has shown that fermented foods, such as yogurt and sauerkraut, can enhance the population of beneficial bacteria. Furthermore, polyphenol-rich foods like berries and green tea have been linked to improved gut microbiota composition. Regular consumption of anti-inflammatory foods can also benefit gut health. Incorporating foods like fatty fish, olive oil, and nuts helps combat inflammation. The Mediterranean diet, for example, has demonstrated positive effects on gut health and metabolic markers. Maintaining a balanced diet not only supports gut health but also promotes insulin sensitivity. Thus, individual dietary choices can significantly influence the gut microbiota and overall metabolic health, making informed choices essential for wellness.
Gut microbiota affects not only metabolic processes but also immune function and inflammation. This link further validates the connection between gut health and insulin resistance. Individuals with insulin resistance often display higher levels of systemic inflammation. Dysregulated immune responses, driven by gut dysbiosis, exacerbate these inflammatory markers. Gut bacteria influence the immune system by interacting with intestinal epithelial cells. For instance, beneficial bacteria can stimulate the production of anti-inflammatory cytokines, while harmful bacteria may trigger pro-inflammatory responses. The health of the gut barrier is critical for maintaining immune balance. A compromised gut barrier, or ‘leaky gut,’ allows toxins to enter the bloodstream, provoking inflammatory reactions. Consequently, addressing gut health may provide a twofold benefit: improving insulin sensitivity and reducing inflammation. In this context, restoring gut balance through dietary choices and probiotics might alleviate insulin resistance. Ongoing research aims to clarify these intricate relationships to better understand how gut health influences metabolic diseases. Engaging in lifestyle changes and considering microbiome-targeted dietary interventions may offer preventive measures against diabetes and other metabolic disorders.
Role of Probiotics and Prebiotics
Probiotics and prebiotics are essential components of a diet aimed at enhancing gut health. Probiotics are live beneficial bacteria that, when consumed, can restore intestinal balance. Prebiotics, on the other hand, are non-digestible fibers that provide nourishment for these probiotic bacteria. Incorporating both into the diet can lead to a healthier gut microbiome, thereby addressing issues like insulin resistance. Research indicates that specific strains of probiotics can help improve insulin sensitivity and reduce fat mass. For example, Lactobacillus and Bifidobacterium strains have shown promising results in studies on metabolic health. Moreover, prebiotic foods such as garlic, onions, and bananas nurture beneficial bacteria, amplifying their positive effects on gut health. This synergy enhances the overall composition of the gut microbiota and can lead to improved glucose metabolism. Choosing foods containing probiotics and prebiotics can create a favorable environment in which beneficial bacteria thrive. Regular consumption of fermented foods, along with fiber-rich fruits and vegetables, enhances gut health. By considering these factors, individuals can take proactive steps in managing their metabolic health effectively.
Monitoring gut health is essential in understanding and managing insulin resistance and related metabolic disorders. Various diagnostic tools, including stool testing, can provide insights into gut microbiota composition. Altered gut microbiota profiles may indicate dysbiosis, guiding appropriate dietary interventions. Through analysis, healthcare providers can tailor recommendations to individual needs. Furthermore, nutrient deficiencies often accompany gut dysbiosis. These deficiencies can impair metabolic function, contributing to insulin resistance. Hence, investigating gut health could influence treatment strategies for diabetes and related conditions. Addressing gut health through personalized nutrition can significantly impact overall metabolic health. For instance, incorporating targeted probiotics and dietary adjustments can lead to tangible improvements in insulin sensitivity markers. Continuous research is exploring the potential of fecal microbiota transplantation as a therapy for metabolic diseases. This innovative approach aims to restore a healthy microbiome through the replacement of dysbiotic flora. Such advancements hold promise for the future of diabetes management. Ongoing studies also investigate the relationship between gut health and other metabolic disorders. These efforts aim to clarify causal relationships, paving the way for effective prevention strategies by promoting gut health.
Stress, Sleep, and Gut Health
Stress and sleep quality are significant factors influencing gut health and may indirectly affect insulin resistance. Chronic stress can alter gut microbiota composition, leading to dysbiosis. This can result in various health issues, including the exacerbation of insulin resistance. Stress triggers the release of cortisol, a hormone that can adversely affect gut bacteria balance. Moreover, poor sleep quality has been connected to increased inflammation and disrupted metabolic regulation, further impacting insulin sensitivity. Therefore, adopting stress management techniques and prioritizing sleep can enhance gut health. Mindfulness practices, including yoga and meditation, promote relaxation and may positively affect gut microbiota. Additionally, ensuring adequate sleep is crucial for hormonal balance and overall metabolic function. Practicing good sleep hygiene, like maintaining a consistent sleeping schedule, can improve gut health indirectly. Emerging research emphasizes the bi-directional relationship between the gut-brain axis and metabolic health. This intricate connection highlights the importance of holistic approaches to health that encompass dietary choices, stress management, and sleep quality. In doing so, individuals can empower themselves to maintain a healthy gut environment.
In summary, the connection between gut dysbiosis and insulin resistance holds significant implications for diabetes management and prevention. Research underscores the importance of maintaining a healthy gut microbiome. Addressing lifestyle factors like diet, stress, and sleep can substantially impact gut health. Promoting dietary diversity rich in prebiotics and probiotics is essential in restoring gut balance. Moreover, understanding individual differences in gut microbiota can help tailor interventions for metabolic disorders. The role of probiotics in enhancing insulin sensitivity and reducing inflammation is equally crucial. Ongoing research into the complex interactions between the gut microbiome and various metabolic pathways will enhance our understanding of diabetes. Future therapeutic strategies may involve personalized nutrition based on gut microbiota profiling. By focusing on gut health, individuals can mitigate the risks associated with insulin resistance and promote overall metabolic well-being. Ultimately, collaborative efforts between healthcare professionals and individuals can foster better health outcomes. As our knowledge deepens, practical applications will emerge, helping to navigate the challenges posed by metabolic diseases like diabetes.