Gut Health and Autoimmune Conditions: Exploring the Link
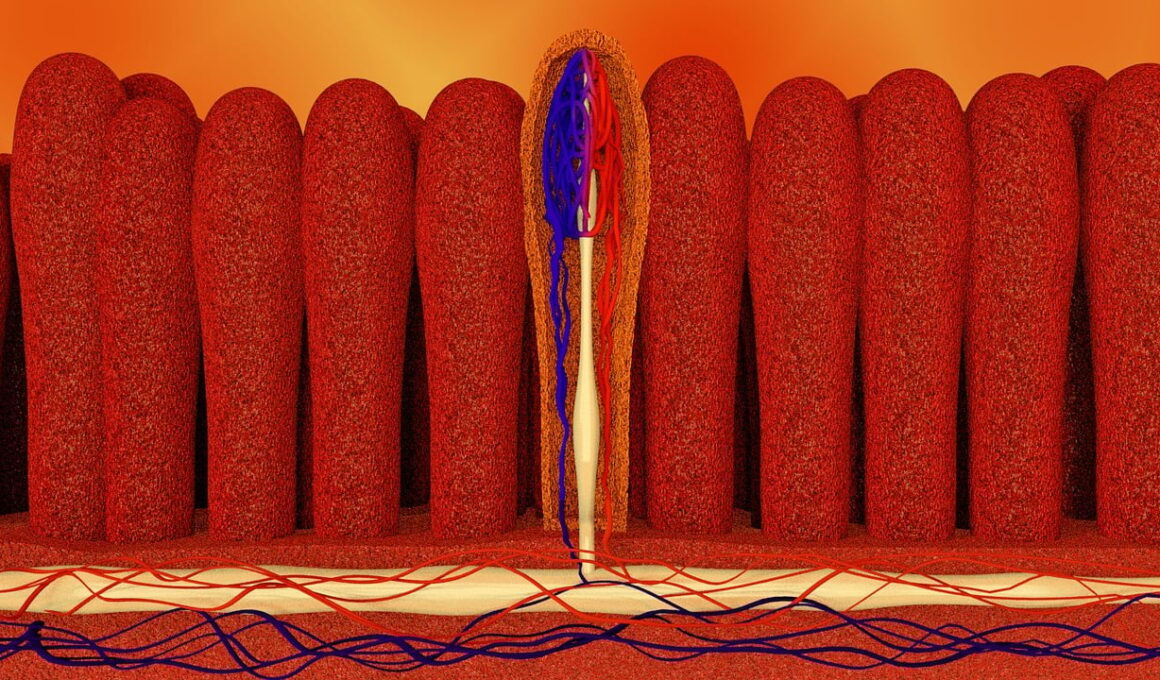
Chronic autoimmune conditions affect millions of individuals worldwide. The connection between gut health and these conditions is increasingly being recognized. Research suggests that a compromised gut barrier, often termed leaky gut syndrome, may play a significant role in the pathogenesis of autoimmune diseases. In leaky gut, the intestinal lining becomes permeable, allowing toxins and undigested food particles to enter the bloodstream. This can trigger systemic inflammation and lead to immune system dysregulation. Studies indicate that addressing gut health can be a crucial component in managing autoimmune diseases. By improving gut integrity through specific dietary interventions and lifestyle changes, many individuals have reported a reduction in their autoimmune symptoms. Healing the gut may involve the addition of fermented foods, rich in probiotics, which can potentially restore gut microbiota diversity. Furthermore, eliminating foods that cause inflammation, such as gluten or dairy, may also be beneficial. Overall, maintaining a healthy gut may be essential for individuals facing autoimmune challenges, underscoring the need for a comprehensive approach to health.
The Gut Microbiome’s Role
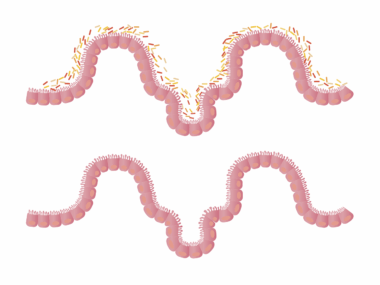
The gut microbiome consists of trillions of microorganisms that play an essential role in human health. This diverse ecosystem influences digestion, immune function, and even mental health. An imbalance in gut microbiota, often referred to as dysbiosis, can lead to various health issues, including autoimmune diseases. Research demonstrates that certain microbiome profiles are linked to the presence of inflammatory markers associated with autoimmune conditions. Therefore, a healthy gut microbiome can contribute to immune system balance and resilience. The introduction of prebiotics, which are dietary fibers that feed beneficial bacteria, may help restore microbiome balance. Including fiber-rich foods such as fruits, vegetables, and whole grains is vital for gut health. Additionally, a diet high in polyphenols, found in colored fruits and vegetables, may support microbial diversity. Lifestyle factors like stress management, adequate sleep, and physical activity also contribute positively to microbiome health. As researchers continue to explore the gut microbiome’s intricate relationships with autoimmune diseases, the holistic approach to gut health becomes even more paramount for prevention and management strategies.
Merging dietary approaches with holistic health practices seems essential for those dealing with autoimmune disorders. Many individuals have turned to diets specifically focused on nurturing their gut, such as the autoimmune protocol (AIP) diet. The AIP diet aims to eliminate inflammation-triggering foods and promote healing through nutrient-dense foods, rich in vitamins and minerals. This process involves removing nightshades, grains, legumes, and processed sugars, emphasizing omega-3 fatty acids, healthy fats, and organic vegetables. Additionally, lifestyle modifications like stress reduction techniques can support gut repair and enhance overall health. Mindfulness, yoga, or meditation may significantly benefit stress management in those facing autoimmune challenges. Restoring balance through these measures not only can improve gut health but also reduce autoimmune symptoms. Many individuals report feeling better after adhering strictly to an AIP diet and integrating stress-relief practices into their daily routines. Remember, individual results may vary, and what works for one person may not work for another. Consulting healthcare professionals significantly understands their unique requirements while exploring dietary and holistic practices.
Nutrients Essential for Gut Health
Certain nutrients are vital for maintaining gut health and potentially mitigating autoimmune conditions. For instance, omega-3 fatty acids are well-known for their anti-inflammatory properties. Sources like fatty fish, flaxseeds, and walnuts can help support a healthy inflammatory response. Additionally, vitamins like A, D, and E play crucial roles in maintaining gut integrity and immune function. Vitamin D, in particular, has been shown to modulate the immune system. By enhancing the gut’s mucosal barrier and regulating inflammation, sufficient vitamin D levels may help reduce the risk of autoimmune diseases. Zinc, another essential mineral, promotes the healing of the intestinal lining and supports immune health. Foods rich in zinc include oysters, pumpkin seeds, and legumes. Lastly, magnesium is involved in various biochemical reactions, including those supporting gut function. Stress management is equally important, as high-stress levels can deplete these nutrients, making their supplementation crucial for individuals struggling with autoimmune conditions. Through dietary adjustments and possibly supplementation, individuals can enhance their gut health and overall well-being.
Hydration also plays an essential role in gut health, particularly when addressing autoimmune issues. Drinking adequate water helps in digestion, nutrient absorption, and waste elimination. Ensuring proper hydration may support the mucous membrane of the gut, which is vital for gut barrier integrity. Herbal teas like ginger or peppermint can also have soothing effects on the digestive system and may ease symptoms that accompany autoimmune diseases. Furthermore, nutrition alone may not be sufficient for managing such conditions effectively. Regular physical activity is equally important, as exercise can promote gut health by enhancing microbial diversity and supporting healthy bowel movements. Even gentle activities like walking or gentle yoga can positively impact gut function. For many, maintaining a balanced lifestyle that incorporates proper hydration, nutrition, and physical movement can create a significant reduction in symptoms. Therefore, consistency in these practices is essential to harness the full advantages in the context of autoimmune conditions. In summary, a comprehensive approach to gut health is invaluable for those looking for relief from autoimmune challenges.
Connection between Inflammation and Gut
Chronic inflammation is a common thread linking autoimmune diseases and poor gut health. Several studies have shown that inflammation can disrupt the gut barrier, further exacerbating health issues. When the intestinal lining is compromised, inflammation can spread throughout the body, potentially leading to the development of autoimmune conditions. Inflammatory bowel conditions, such as Crohn’s disease or ulcerative colitis, demonstrate this link clearly, signaling how poor gut health may contribute to autoimmune reactions. Those suffering from inflammation-related symptoms should prioritize their diets even more. Utilizing anti-inflammatory foods, including leafy greens, berries, and fatty fish, can benefit gut healing. Furthermore, removing foods that tend to trigger inflammation, like refined sugars and processed foods, is paramount for overall health. As an approach, minding portion sizes can also help avoid overloading the digestive system, reducing inflammation further. Collaboratively using anti-inflammatory diets and lifestyle choices may provide a solid foundation for managing autoimmune conditions effectively. Education and awareness in nutrition play crucial roles in fostering better digestive health and reducing inflammation across the population.
Lastly, a supportive community and resources for individuals navigating autoimmune diseases cannot be underestimated. Platforms that encourage sharing experiences and strategies can be incredibly beneficial. Individuals may find solace in connection with others aware of their struggles. Social interactions can significantly influence stress levels, making emotional support crucial in holistic health approaches. There are various online forums, local health groups, and resources dedicated to people with autoimmune conditions. Seeking out professionals knowledgeable in integrative health can also provide personalized guidance as individuals embark on their healing journeys. Healthcare providers who consider both conventional and holistic approaches can offer a well-rounded perspective on tackling autoimmune issues. Staying informed and proactive empowers individuals to take charge of their health. Adapting lifestyle habits and dietary changes may not always be easy, but the potential benefits to gut health and overall well-being are encouraging. In conclusion, the intricate connection between gut health and autoimmune conditions highlights the importance of holistic approaches, encompassing nutrition, lifestyle choices, and community support.
Future Directions in Research
The ongoing search to understand the dynamic relationship between gut health and autoimmune conditions represents an exciting frontier in health research. As scientists uncover the roles of genetics, environment, and microbiome interaction, more knowledge can lead to innovative treatments. Potential therapies may involve personalized nutrition plans tailored to individual microbiome profiles, thereby enhancing effectiveness. Advanced technologies, such as gut microbiome testing, hold promise for customizing dietary interventions. Additionally, the focus on preventive strategies aimed at supporting gut barrier integrity before autoimmune symptoms manifest may significantly influence the future of health management. Exploring the effects of lifestyle factors, such as adequate sleep, stress management, and physical activity, also remains critical in future studies. Investing in research dedicated to gut health will streamline approaches to addressing not only autoimmune conditions but overall health. Patients and healthcare providers will benefit from clearer guidelines and evidence-based protocols, ensuring that integrative health strategies become a priority. By pushing the boundaries of scientific inquiry, there is potential to reshape the landscape of healthcare, forging connections between seemingly disparate elements of health. Therefore, advocating for investment in this research arena is essential for transformative healthcare improvements.