The Importance of Early Microbial Exposure in Allergic Disease Development
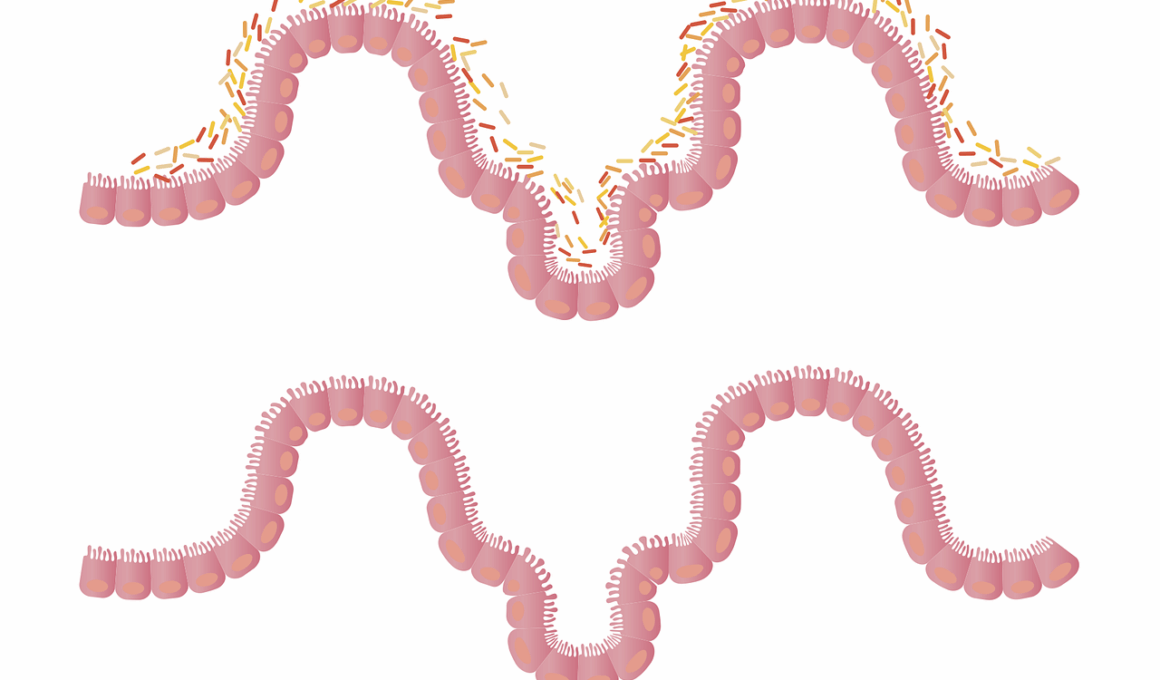
Emerging research underscores the crucial role of the gut microbiome in the development of allergic diseases. The gut microbiome consists of a diverse community of microorganisms that contributes significantly to human health. Early microbial exposure is becoming increasingly recognized as a key factor in modulating immune responses, particularly in infants. The hygiene hypothesis suggests that reduced microbial exposure leads to an increased prevalence of allergies in modern societies. Factors such as urban living, reduced family size, and increased use of antibiotics diminish microbial diversity. These factors can result in an altered gut microbiota composition, which may contribute to inappropriate immune responses. Moreover, the timing of microbial exposure may shape the diversity of gut flora, impacting the immune system’s development. This complex interplay between gut microbiome and the immune system is critical. Additionally, specific microbial species have been linked to protective effects against allergies. Understanding these dynamics could lead to novel strategies for preventing allergic diseases, especially through interventions that promote microbial richness early in life, ensuring adequate immune training and reducing the incidence of allergic reactions.
Understanding Allergic Disease Development
Allergic diseases are prevalent conditions that significantly affect the quality of life of millions worldwide. They arise from hypersensitive immune responses to normally harmless substances, known as allergens. Common allergic conditions include asthma, allergic rhinitis, and food allergies. The exact triggers for allergic diseases are multifactorial, influenced by genetic predisposition, environmental exposures, and indeed, the gut microbiome. Studies have shown that an imbalanced microbiome can negatively affect immune system development and function. Infants with a diverse gut microbiome composed of beneficial bacteria tend to exhibit lower rates of allergies. In contrast, those with reduced microbial diversity are more susceptible to allergic manifestations. The interactions between specific gut microbiota and innate immune system components can drive these immune responses. Identifying beneficial microorganisms and understanding mechanisms through which they exert protective effects against allergies provide avenues for treatment and prevention. Furthermore, early dietary interventions focused on exposing infants to specific bacteria and prebiotics might help enhance microbial diversity, potentially offering long-term benefits in allergic disease management and prevention.
Breastfeeding plays a key role in shaping the infant gut microbiome and potentially reducing allergies. Breast milk is rich in prebiotics, providing essential nutrients for gut bacteria. These nutrients facilitate the growth of beneficial microbes, contributing to a healthy gut environment. Studies indicate that infants who are exclusively breastfed have a lower risk of developing allergic diseases compared to formula-fed infants. The composition of breast milk is dynamic, adapting to the infant’s needs and promoting a diverse gut microbiome. This process can also influence T-cell differentiation and the immune system’s response to allergens. Introducing solid foods too early or too late can disrupt this delicate balance, potentially triggering allergic reactions. The timing and type of food introduction can shape the gut microbial community. Fermented foods that contain live bacteria may be particularly beneficial. Parents should consider delaying common allergens, such as peanuts and eggs, in their infants’ diets while ensuring a diverse intake of foods. Collaborative efforts between healthcare providers and families are crucial for establishing guidelines about dietary practices that foster microbial health, reducing allergy prevalence.
Environmental Factors Influencing Gut Microbiome
The environment in which a child grows up can significantly impact microbial exposure and gut health. Urbanization, dietary patterns, and antibiotic use are major factors influencing gut microbiome diversity. Children raised in rural areas tend to have greater exposure to a wider range of microbes, which may protect against allergies. Pets in the home can also introduce beneficial microorganisms, enhancing microbial diversity and possibly reducing allergic responses. Conversely, urban living often limits microbial exposure due to cleaner environments and diminished interactions with nature. Artificial environments restrict access to beneficial microbes, leading to a less diverse microbiome. Moreover, over-prescription of antibiotics can be detrimental to the gut microbiome. Antibiotics can alter microbial composition, killing off not only harmful bacteria but also beneficial ones. This disruption can have lasting effects on health, including susceptibility to allergic diseases. Therefore, mindful use of medications and embracing a lifestyle that promotes microbial diversity are essential. Engaging with nature, consuming diverse diets, and limiting unnecessary antibiotic use can all contribute to a healthier gut microbiome and reduce allergic disease risks.
Research continues to explore the promising link between probiotics and allergic disease prevention. Probiotics are live microorganisms that confer health benefits when consumed adequately. These beneficial bacteria have demonstrated potential in restoring balance in the gut microbiome and enhancing immune function. Specific strains, such as Lactobacillus rhamnosus, may help alleviate allergy symptoms when administered during pregnancy, lactation, or infancy. Probiotics may assist in modulating immune responses by promoting the production of regulatory T-cells. Their role in reducing inflammation and bolstering gut health has been well-documented. However, not all probiotics are created equal, and efficacy can depend on strain, dosage, and individual patient factors. Therefore, personalized approaches to probiotic supplementation may prove most effective. Clinical trials are underway to assess the efficacy of specific probiotic strains in preventing allergic diseases. It is paramount that parents and healthcare providers remain informed about these developments. The integration of probiotics into dietary plans could provide a tangible strategy for reducing allergy incidence, particularly in those children at higher risk due to their family histories and environmental exposures.
The Future of Allergy Prevention and Microbial Research
The future of allergy prevention lies in a more profound understanding of the gut microbiome and its critical role in immune system development. As research advances, targeted interventions may emerge that harness the power of microbes to promote better health outcomes. Techniques to analyze the microbiome such as shotgun metagenomics and advanced sequencing technology have enhanced our understanding considerably, making personalized microbiome therapy a real possibility. Exploring how individualized dietary strategies can optimize gut flora without affecting the current microbial balance is essential. Future studies will likely aim at discovering new strains of bacteria that could be beneficial in allergy prevention. Furthermore, creating guidelines for optimal microbial exposure during pregnancy and early childhood might significantly impact allergic disease rates. Parents, healthcare professionals, and policymakers need to work collaboratively to promote environments conducive to microbial diversity. Education surrounding dietary choices and microbial health can empower families to make informed decisions. This proactive approach has the potential not just to reduce allergies, but also to improve overall public health standards, benefiting future generations.
In conclusion, the evidence linking gut microbiome health to allergic disease development is robust and rapidly evolving. Promoting early microbial exposure through breastfeeding, dietary diversity, and healthy environmental practices is imperative. This approach could dramatically lessen the burden of allergic conditions. As our understanding of the microbiome grows, so do the possibilities for prevention strategies that alter the course of allergic disease. Given the potential for probiotics and dietary treatments, individuals may gain proactive tools to combat allergies. Strengthening the gut microbiome must become a focal point in public health initiatives. Moreover, collaborative research across disciplines, including immunology, microbiology, and nutrition, will be vital. By investing in microbiome health from an early age, we can improve the immune development and potentially curb the rising rates of allergies worldwide. Adapting lifestyle choices and fostering a microbial-rich environment may serve as powerful weapons against allergic diseases, creating healthier futures for individuals across the globe. As ongoing effort and research unveil new strategies, the promise of a healthier tomorrow becomes increasingly attainable.