The Effect of Antibiotics on Gut Health in Autistic Individuals
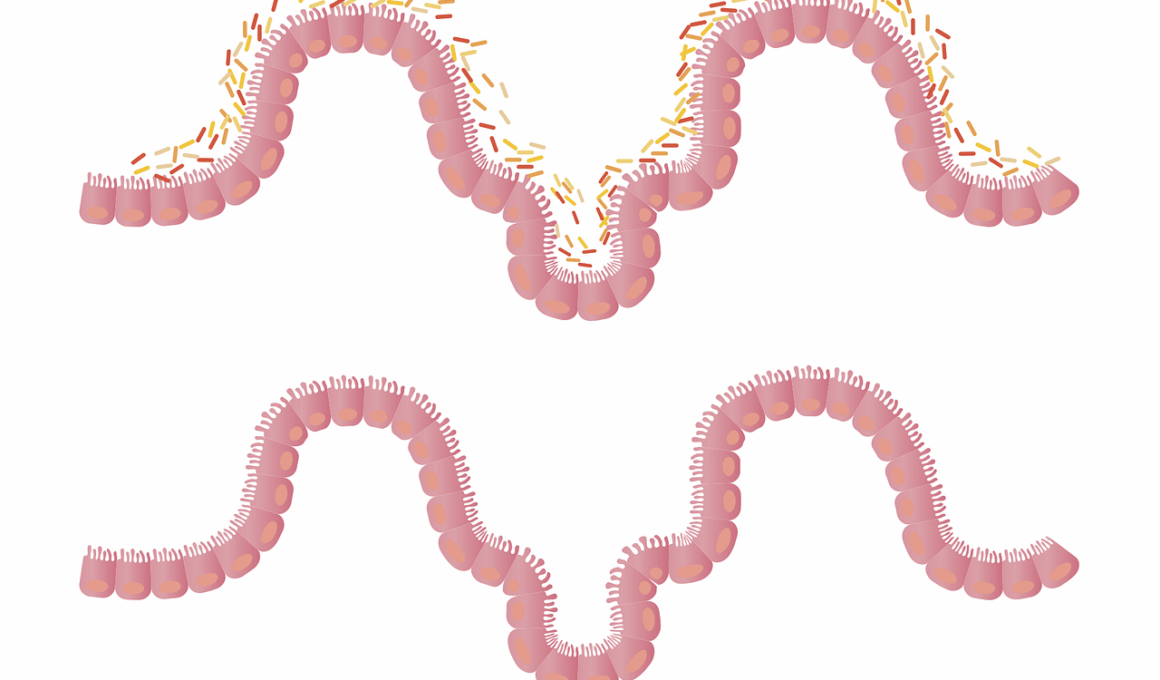
The human gut microbiome consists of trillions of microorganisms, including bacteria, that play a vital role in health. Among various health conditions, autism spectrum disorder (ASD) has drawn attention concerning gut health. Recent studies suggest a connection between gut microbiota imbalance and autism symptoms. Researchers emphasize the need to explore the effects of antibiotics on gut microbiome in autistic individuals. Antibiotics can disrupt the delicate balance of gut bacteria, and this dysbiosis may aggravate existing issues in autistic individuals. Some studies indicate that individuals with ASD often display gastrointestinal abnormalities, further complicating their condition. The microbiome’s role in producing neurotransmitters and regulating immune responses may influence not only gut health but also behavior. As such, understanding the antibiotic influence is paramount. Challenges arise, however, due to the variability of individuals on the autism spectrum. This variability results in diverse immune responses and microbiome composition, leading to varying reactions to antibiotics. Therefore, targeted research is crucial to understand these nuances and compensate for factors like genetic predispositions and environmental exposures.
Antibiotics and Microbiome Dysbiosis
Antibiotics are designed to combat bacterial infections; however, their use can lead to microbiome dysbiosis. Dysbiosis refers to an imbalance in the microbial community that can cause negative health effects. For autistic individuals, dysbiosis might contribute to worsening gastrointestinal symptoms. Research reveals that many ASD patients report digestive issues, suggesting that such imbalances can worsen their condition. Frequent use of antibiotics can lead to a decrease in microbial diversity, which is essential for maintaining gut health. Occasional antibiotic exposure might not exhibit significant immediate side effects, yet the cumulative effect over time could be concerning. Notably, studies indicate that certain gut bacteria play roles in neurodevelopment and cognitive functions. For autistic individuals, maintaining a diverse microbiome might help in managing symptoms better than relying solely on antibiotics for treatment. Given the critical nature of microbial exposure on the immune system, it becomes vital to evaluate each antibiotic’s impact uniquely. Healthcare providers should consider the patient’s medical history and lifestyle, as well as alternatives to antibiotics when possible, in managing infections in autistic patients.
As scientists explore the relationship between gut health and autism, diet emerges as a significant factor. Nutritional choices play a vital role in shaping the gut microbiome. Diets rich in fiber support healthy bacterial growth, which can potentially counteract the adverse effects of antibiotics. For autistic children, incorporating foods such as fruits, vegetables, and whole grains may help restore balance in gut microbiota. Moreover, probiotics, often consumed through fermented foods or supplements, can provide beneficial bacteria that help mitigate dysbiosis following antibiotic treatment. Parents and caregivers should work with nutritionists to devise feeding strategies that support gut health. Identifying allergens or food sensitivities is also essential, as improper foods can exacerbate GI symptoms. Balancing antibiotic use with dietary choices requires mindfulness from caregivers, signifying a necessary collaboration between medical and nutritional teams. Regular monitoring of responses to dietary adjustments is essential in maximizing therapeutic potential. This strategy may enhance overall well-being while addressing the core concerns associated with antibiotics. Additionally, parental education on nutrition can empower families to take an informed stance on managing gut health collaboratively.
The Role of Prebiotics and Probiotics
Recent attention has shifted towards the potential of probiotics and prebiotics in ameliorating gut health. Probiotics, which are live beneficial bacteria, can enhance gut microbial balance post-antibiotic treatment. Conversely, prebiotics are substances that promote the growth of these beneficial bacteria. Scientific evidence supports that incorporating diverse probiotics may alleviate gastrointestinal symptoms associated with antibiotic use. Clinical trials have shown promising results when autistic individuals receive probiotics. Symptoms such as constipation or diarrhea exhibited improved outcomes. While clinical understanding remains incomplete, preliminary findings suggest that increasing healthy microbial populations can lead to better gut health. The objectives herein are to support overall health, reduce inflammation, and possibly decrease behavioral symptoms associated with autism. It’s vital that healthcare providers recommend clinically tested strains of probiotics tailored to individual needs. According to recent studies, dietary components can work synergistically with selected probiotics, creating a health-promoting environment within the gut. Potentially addressing both core and secondary autism symptoms requires a more holistic approach with continued research in microbiome-targeted therapies.
Furthermore, observing individual responses to dietary changes, probiotics, and antibiotics reveals critical insights into holistic care. Personalized medicine is pivotal, as ASD presents uniquely in each individual. This personalized approach can lead to better health outcomes, emphasizing the necessity for tailored interventions. Health professionals must remain vigilant in monitoring each individual’s reaction to these treatments, ensuring comprehensive assessments are in place. A multidisciplinary approach involving physicians, nutritionists, and therapists is crucial in understanding the combined effect of antibiotics, diet changes, and supplements on gut health. It empowers families with knowledge and resources, helping to navigate the complexities associated with ASD. Ongoing communication is key; regular follow-ups can reveal emerging patterns and effects that might go unnoticed otherwise. Additionally, this collaborative effort can facilitate the identification of triggers that exacerbate gut issues in autistic individuals. Continuous education surrounding the gut-brain connection can aid in optimizing interventions that enhance quality of life. As research continues to unfold, it is essential that personalized treatment plans adapt to these new findings, ensuring that autistic individuals receive the best care tailored to their needs.
Conclusion and Future Directions
In conclusion, exploring the effect of antibiotics on gut health in autistic individuals remains a vital area of research. Given the evidence linking gut microbiome changes and autism spectrum disorder, addressing gut health through responsible antibiotic use and dietary interventions emerges as critical. Importantly, integrating probiotics and prebiotics offers a promising strategy to counteract dysbiosis and improve health outcomes. Future studies should focus on larger, diverse samples to establish the most effective approaches for promoting gut health among individuals with ASD. Developing specific guidelines for using antibiotics and concurrent therapies can create consistency in treatment protocols, empowering healthcare providers to support families better. Conclusively, fostering awareness of these connections among caregivers, healthcare professionals, and researchers could transform management strategies for autism effectively. Impactful changes can arise from informed dietary choices and strategic antibiotic use. This area shows promise but requires commitment and study to unravel complexities related to autism and gut health profoundly. The journey towards better health outcomes must involve reflection upon intervention strategies as researchers advance their understanding of the gut-brain axis.
Ultimately, the objective remains enhancing the quality of life for autistic individuals through focused and individualized interventions. The potential of understanding the gut microbiome holistically continues to evolve, revealing exciting opportunities for treatment advancements. Continued research into the interplay between antibiotic use, gut microbiome health, and autism will not only shed light on existing theories but also pave the way for groundbreaking therapies. Encouraging interdisciplinary collaboration among different fields will strengthen the understanding of microbiome dynamics, leading to innovative solutions. It is paramount that all stakeholders remain engaged in discussing and disseminating findings, as the impact of these discoveries transcends academia and enters communities. As we strive for better care and outcomes, fostering dialogue among researchers, clinicians, and families will be key in creating effective strategies. Together, they can ensure that autistic individuals receive the support they deserve. Awareness initiatives can empower families with knowledge and tools to make informed decisions pertaining to their loved one’s health. The ultimate goal is to cultivate healthy gut microbiomes while mitigating the adverse effects of antibiotics, thereby nurturing better developmental and behavioral outcomes.