Tips for Storing Diabetes Medications Safely During Emergencies
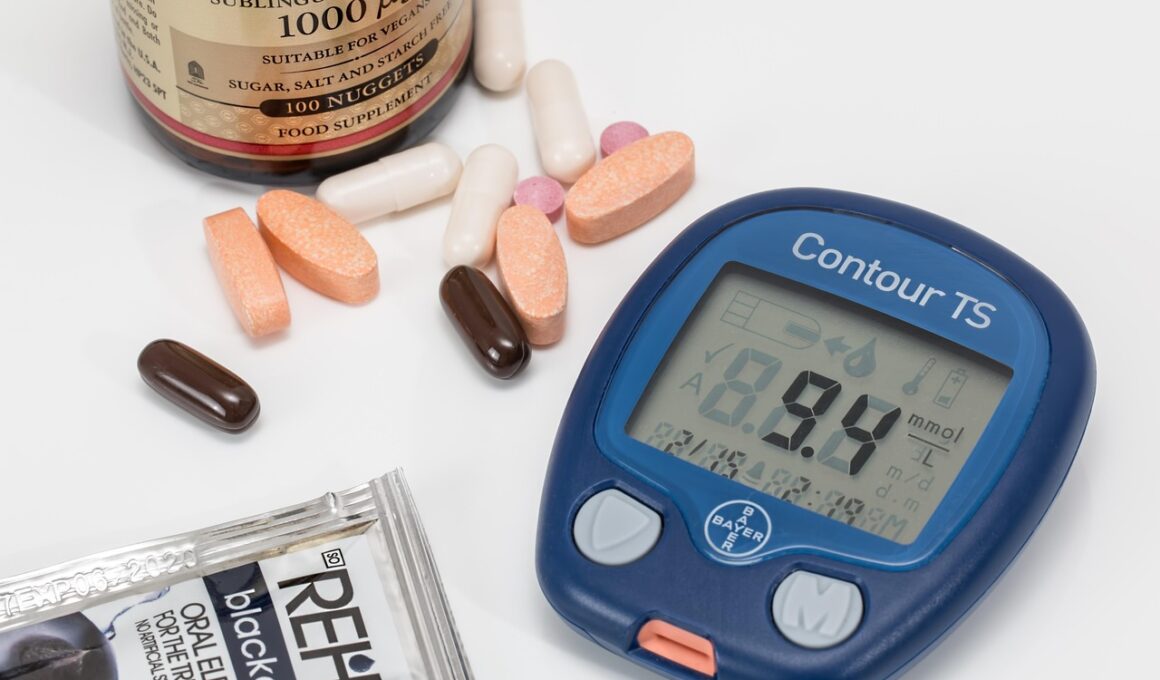
Being prepared for emergencies is crucial for diabetics, as proper medication storage can significantly impact health outcomes. First, it’s vital to understand that many diabetes medications, including insulin, require specific storage conditions. Insulin should be kept refrigerated, but can also be stored at room temperature for a limited period. Make sure to check the manufacturer’s guidelines for each medication. Additionally, create a medication management plan that includes a list of all prescribed items. This list will ensure you have everything you need in an emergency and can also assist caregivers. Moreover, consider the potential loss of power during emergencies. Thus, it is advisable to have backup cooling options available, like ice packs in insulated bags. Regularly monitor expiration dates on medications to avoid using ineffective products. Last but not least, inform family and friends about your medication needs to ensure they assist you effectively in case of an emergency. Having a dedicated storage container that is waterproof and durable helps protect medications from damage during unforeseen situations, ensuring your health remains a top priority.
Another essential aspect of diabetes preparedness includes keeping an emergency kit ready. This kit should contain not only medications but also essential supplies such as blood sugar monitors, testing strips, and dietary snacks. It is crucial to check the kit periodically to ensure that supplies are intact and not expired. Include a copy of your medical history and a list of your medications in this kit. This information can be invaluable if you need medical assistance during a crisis. Furthermore, label all your medications with clear instructions on how to administer them, including dosages. This will not only help you but also others who might assist you in your care. If you plan to travel, take extra supplies and medications to cover potential delays. Staying organized can alleviate stress in emergencies and allow quick access to necessary items. Empower yourself and your loved ones with knowledge about recognizing and treating low or high blood sugar levels in emergencies. Knowing how to handle these situations can save lives and ensure you remain stable until more help is available.
Educate Yourself and Others
Education plays a key role in diabetes and emergency preparedness. Understanding your condition and how various emergencies can impact it will help you make informed decisions. Attend workshops or training sessions related to diabetes management. Share this knowledge with family and friends so they can provide better support when needed. Practical exercises, like simulating emergency situations, can prepare everyone involved. This training can help reinforce the information so it’s retained long-term. It’s also helpful to create an emergency action plan which includes steps to take during different emergencies, including natural disasters. Distributing this plan among your family members and caregivers ensures everyone is on the same page regarding your diabetes management. Engage with local diabetes support groups or associations for additional resources and information. They often provide materials that can help people better prepare for emergencies. Additionally, familiarize yourself with local health facilities and their emergency protocols. These steps will empower you and your support network, ensuring that diabetes care remains consistent during emergencies. Remember, preparation and education are the keys to safety for diabetics in crisis situations.
Another critical element in managing diabetes during emergencies involves communication. Always carry an identification card indicating your diabetes status and necessary medications. This helps first responders understand your medical needs, thus improving the care you receive. It’s advisable to have a list of emergency contacts readily available, including healthcare providers. Keep this list in your emergency kit for quick access. Furthermore, check with your healthcare provider about recommendations specific to your circumstances, such as dosage adjustments. This is particularly important if you are on medication that could affect your ability to endure heat or cold during emergencies. Store your medications in a climate-controlled environment whenever possible. Extreme temperatures can affect their efficacy, especially in hot weather or during winter storms. Aim to have a backup plan for accessing medications when pharmacies may be closed or unavailable. This may involve establishing relationships with multiple pharmacies or obtaining an extra supply from your healthcare provider. Staying proactive with communication ensures that your diabetes management plan remains a priority regardless of the situation.
Alternative Power Source Considerations
In many emergency situations, power loss is a significant concern, especially for diabetics who rely on insulin storage. Consider acquiring a portable generator or a car inverter to keep medications at the right temperature. These devices can be invaluable during extended power outages due to storms or natural disasters. Additionally, utilize coolers with ice packs as a temporary measure to preserve insulin effectively for several hours. If you can maintain a steady power supply, ensure your devices are fully charged and ready for use. It’s also advisable to have a power bank for your electronic devices to ensure continuous accessibility to your diabetes management app and appointments. When developing your emergency preparedness plan, consider integrating a buddy system with a friend or family member who also understands your diabetes needs. They can help monitor your condition or assist with medication administration in emergencies. Furthermore, connect with local community resources so that they can help you in times of need. Collaboration during emergencies can streamline your diabetes care effectively, providing peace of mind.
Paying attention to your diet during emergencies is just as crucial as managing medications. Ensure that your emergency food stash includes low-glycemic snacks and quick carbohydrates to address sudden blood sugar changes efficiently. Maintain food items that are easy to store and prepare, such as canned or freeze-dried meals. Additionally, keep a small supply of protein bars or shakes available for convenience. Label all food items clearly to avoid confusion in a hurry. During emergencies, it’s essential to have non-perishable foods that provide nutritional benefits. Remember to include enough fluids for hydration, as stress can cause dehydration, making blood sugar management even more challenging. Check regularly for any food items in your emergency kit that may expire soon and replenish them as required. Consider storing additional dietary materials, like sugar-free or gluten-free options if needed. Keeping your nutrition in mind ensures that you remain healthy and stable, ultimately aiding you in managing your diabetes during crises. Preparedness in dietary supplies can significantly enhance your quality of life during challenging situations.
Review and Reassess Your Plan
After creating a diabetes emergency preparedness plan, it’s essential to periodically review and update it. Situations change, and so can your medication needs or lifestyle. Schedule regular check-ins, ideally every six months, with your healthcare provider. This ensures that all medications are accounted for and are still suitable. During these discussions, reassess your storage needs as well. Are you still using the same devices and supplies? Have there been any advancements in diabetes medications or technology? Additionally, pay attention to the feedback from family and friends regarding your preparedness plan. Their insights can provide valuable information on what may need improvement, ensuring that your plan remains comprehensive. If you encounter any new challenges or discover additional support systems, integrate that into your plan. An adaptable and thorough preparedness approach can enhance the support you receive during emergencies. Keeping communication open with loved ones will solidify your emergency management strategy, maximizing safety during crises informed by ongoing updates about your condition. Ultimately, being proactive can save time, reduce stress, and can lead to better health outcomes during emergencies.
In conclusion, the importance of emergency preparedness for diabetics cannot be understated. By regularly reviewing medications and supplies, creating thorough plans, and keeping open lines of communication with your support network, you position yourself for success during emergencies. It’s crucial to understand your individual needs and how they relate to emergency scenarios. Taking proactive steps enables you to react promptly and efficiently when faced with unexpected challenges. Investing time into preparing your medication storage, communication, and educational components will establish a solid foundation for effective diabetes management. As emergencies can arise at any moment, don’t wait until a crisis occurs to prepare for it. Knowing your medication needs, having access to necessary supplies, and being educated about managing diabetes effectively ensures that your health remains a priority. Each of these strategies contribute to maintaining stable blood sugar levels during unexpected situations. Therefore, treat preparedness as an ongoing journey, consistently evolving, and adapting to new information or changes in your health status. Equip yourself adequately, and you will significantly improve resilience in the face of emergencies.