Medications Impacting Gut Barrier Function and Microbiome Health
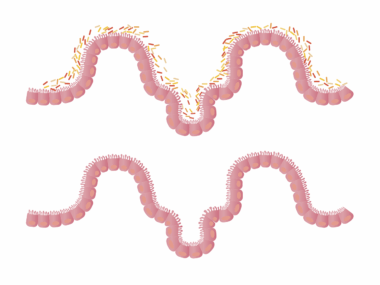
The gut microbiome plays a crucial role in overall health, regulating digestion and immune function. It is significantly influenced by various factors, particularly medications. Some medications can disrupt the gut microbiome’s delicate balance, leading to potential health issues. Antibiotics, for instance, are known for their powerful ability to combat infections, yet they also target beneficial bacteria in the gut. When beneficial bacteria are diminished, the gut barrier function becomes compromised, leading to increased permeability or leaky gut. This situation allows toxins and undigested food particles to enter the bloodstream, which can trigger inflammatory responses and contribute to various gastrointestinal conditions. Chronic use of medications such as non-steroidal anti-inflammatory drugs (NSAIDs) can further exacerbate this issue by irritating the gut lining and altering microbiome diversity. Understanding the impact of medications is vital, as it helps reinforce the importance of cautious use and monitoring. Health professionals need to consider not only the benefits of medications but also their potential risks on gut health. Patients should be informed about these factors to ensure they make well-informed decisions regarding their treatments.
Another category of medications impacting gut microbiome health are proton pump inhibitors (PPIs). These widely used medications reduce stomach acid, which is fundamental for digestion and absorption of nutrients. While PPIs offer relief from conditions like gastroesophageal reflux disease (GERD), prolonged use can lead to gastrointestinal disturbances. Reduced acidity in the stomach allows for the overgrowth of pathogenic bacteria in the intestines, further disrupting the balance of the microbiome. This imbalance may manifest as symptoms such as bloating, diarrhea, or more serious gastrointestinal infections. Research also suggests a potential link between chronic PPI use and various gastrointestinal disorders. Patients using these medications should regularly consult their healthcare providers to evaluate their necessity and explore alternative treatment options. The decision to continue PPIs must weigh potential gut health risks against their benefits. Exploring dietary approaches or lifestyle changes may offer a safer route to manage symptoms. Collaborative approaches between patients and providers can enhance understanding and mitigate risks associated with long-term medication use, ultimately fostering healthier gut environments. This mindful approach is essential to support gut microbiome resilience and functioning.
Antibiotics, as discussed earlier, significantly affect gut microbiota, fundamentally changing the composition of microbial communities. While they contribute toward eradicating harmful bacteria, they also wipe out beneficial strains that play protective roles in gut health. This disruption can lead not only to acute digestive disturbances but also to long-term complications such as antibiotic-associated diarrhea or Clostridium difficile infections. The altered microbiota may take time to recover, and in some cases, restoration of the original microbiome composition might not be achieved. Patients given antibiotics should be aware of the possible necessity of probiotic supplementation following treatment. Probiotics may help re-establish a healthy balance by replenishing beneficial bacteria lost during antibiotic use. Dietary choices also matter—consuming fiber-rich foods supports the growth of beneficial gut bacteria, promoting recovery. Educating patients on dietary strategies and possible supplementation can enhance the overall therapy. Integrative strategies help promote effective recovery and reduce the risk of complications associated with antibiotics. Understanding this relationship can guide appropriate interventions to support gut microbiome restoration, enhancing patients’ long-term health outcomes.
Long-term Medications and Gut Health
The impact of long-term medications on gut microbiome health cannot be understated. Various chronic conditions require ongoing treatments that may inadvertently affect gut health over time. Medications such as corticosteroids, commonly used for their anti-inflammatory effects, can alter the gut microbiota. Research indicates that these medications might play a role in increasing the risk of infections like Clostridium difficile. Corticosteroids can also impact the immune response, leading to increased gut permeability. Furthermore, medications aimed at treating psychiatric disorders, such as antidepressants, may influence gut health by interacting with the gut-brain axis. A disturbed microbiome could potentially affect emotional and mental well-being. Patients undergoing long-term medication regimens should be routinely assessed for potential impacts on their gut health. Healthcare providers may consider alternative therapies, lifestyle modifications, or regular monitoring to minimize risks. Education about the side effects of medications is crucial for patients, allowing them to engage meaningfully in their health management. Through this, providers can derive strategies that help mitigate gut-related complications from chronic medications. Supporting the gut microbiome could enhance their overall health and treatment success.
Medications that directly influence gut motility also warrant attention. Laxatives, frequently prescribed for chronic constipation, may lead to imbalances in gut microbiota if used excessively. When the gut is consistently stimulated by laxatives, it can disrupt normal bacterial assembly and lead to dependency on the medication for bowel movements. Such dependencies might result in diminished gut contractions over time, leading to further digestive challenges. Educating patients about the potential long-term effects of laxative misuse is essential. Strategies aimed at improving stool consistency and promoting natural bowel movements should be encouraged over extended laxative use. Increasing dietary fiber intake, ensuring proper hydration, and engaging in regular physical activity can contribute to better bowel health without the adverse effects associated with laxatives. Patients must understand that restoring healthy bowel function may require a gradual approach towards dietary and lifestyle corrections. Addressing the underlying causes of constipation, alongside medications, can foster a healthier gut environment. Empowering patients with knowledge on the appropriate use of laxatives can effectively support their digestive health.
Herbal and Supplement Interactions
Additionally, the intersection of herbal supplements and prescribed medications may pose risks to gut health. Patients often turn to herbal remedies for various reasons, including gastrointestinal discomfort. However, some herbs can potentially interact with drugs, altering their effectiveness or leading to adverse effects. For instance, certain herbal supplements can impact the metabolism of medications processed in the liver, changing their concentrations and efficacy. The digestive system is responsible for absorption and enzymatic breakdown, making it vulnerable to influences from both medications and supplements. Healthcare providers should inquire about herbal supplement use when prescribing medications to ensure safe combinations. Furthermore, not all herbal supplements undergo rigorous testing, raising concerns about quality and consistency. Patients must be guided on seeking reputable sources when considering herbal alternatives, knowing that natural does not always equal safe. Clear communication between patients and providers is key in navigating these interactions, fostering informed decisions. Empowering patients with comprehensive knowledge on herbal-supplement-drug interactions can safeguard their gut health, contributing to more effective treatment plans.
Overall, enhancing awareness of the relationship between medications and gut microbiome health is vital. Patients and healthcare providers share responsibility in optimizing gut health while managing medical conditions. Proper education regarding the effects of different medications can help promote better communication and safer usage. Patients should engage actively with their healthcare providers, discussing any concerns about their gut health related to their medications. Additionally, integrating dietary and lifestyle changes can support gut integrity during treatments. Proactive measures, such as considering probiotics and prebiotics, may bolster the microbiome in situations of medication-induced disruption. Health experts should advocate for developing strategies to minimize negative impacts on the gut, ensuring patients have avenues for recovery. Ultimately, adopting a holistic approach that considers both medication effects and overall gut health can lead to improved patient outcomes. Building a strong foundation for gut microbiome health is essential, contributing to optimal health across all systems. By prioritizing this connection, medical practitioners can help patients achieve a balanced and healthy gut microbiome that supports their well-being.
Conclusion
In conclusion, understanding the medications that impact gut barrier function is essential for promoting microbiome health. From antibiotics to long-term medications, each can affect the gut microbiota. Educating patients about these effects encourages smarter medication use, better dietary choices, and overall lifestyle modifications. Patients must become active participants in their health journeys, advocating for their gut health. Collaborative efforts among healthcare providers and patients can lead to innovative strategies to minimize the adverse effects of medications. This proactive approach fosters a holistic understanding of gut health, considering all factors influencing it. Utilizing evidence-based practices enhances recovery processes and promotes better health. Most importantly, making informed decisions ensures that patients can enjoy the benefits of their medications while minimizing potential risks. It is imperative to shift the focus towards maintaining a healthy gut microbiome, as it plays a critical role in the overall well-being. A well-balanced microbiome can contribute to reduced inflammation and enhance immune functions. Continuing research related to medications and their impact on gut health will provide valuable insights. A dedicated effort from all angles will ensure the promotion of gut health in the medical community.